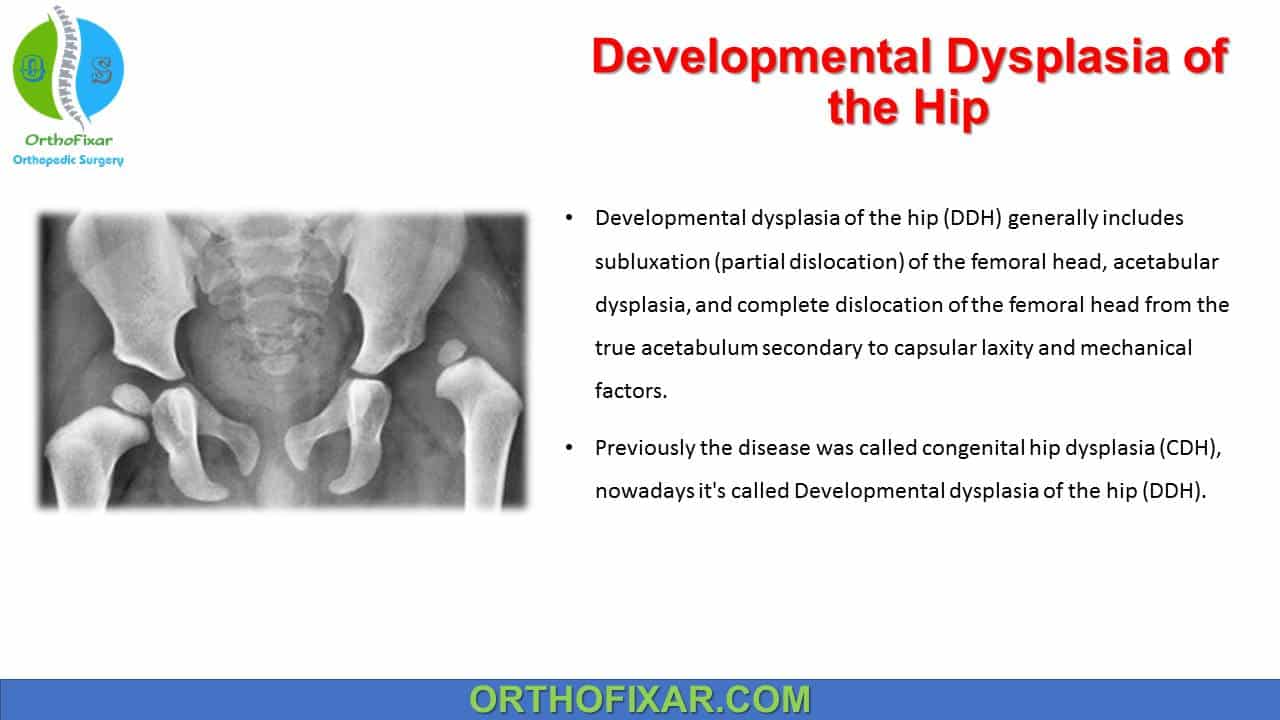
Developmental dysplasia of the hip (DDH) generally includes subluxation (partial dislocation) of the femoral head, acetabular dysplasia, and complete dislocation of the femoral head from the true acetabulum secondary to capsular laxity and mechanical factors.
Previously the disease was called congenital hip dysplasia (CDH), nowadays it’s called Developmental dysplasia of the hip (DDH).
The word developmental invokes the dimension of time, acknowledging that the dysplasia or dislocation may occur before or after birth, while dysplasia means an abnormality of development and encompasses a wide spectrum of hip problems.
Definitions
Instability is the inability of the hip to resist an externally applied force without developing a subluxation or dislocation.
A subluxation is an incomplete dislocation with some residual contact between the femoral head and acetabulum.
A dislocation indicates complete displacement of the femoral head from the acetabulum.
Epidemiology
The incidence of developmental dysplasia of the hip has been estimated to be approximately 1 in 1000 live births. It’s more common in girls (85%).
It’s most often in the left hip (67% of cases), and bilateral involvement is more common than involvement of the right hip alone.
The incidence in infants with a positive family history is ≥20%.
The incidence in the presence of increased maternal estrogens, and in breech births (30% to 50%).
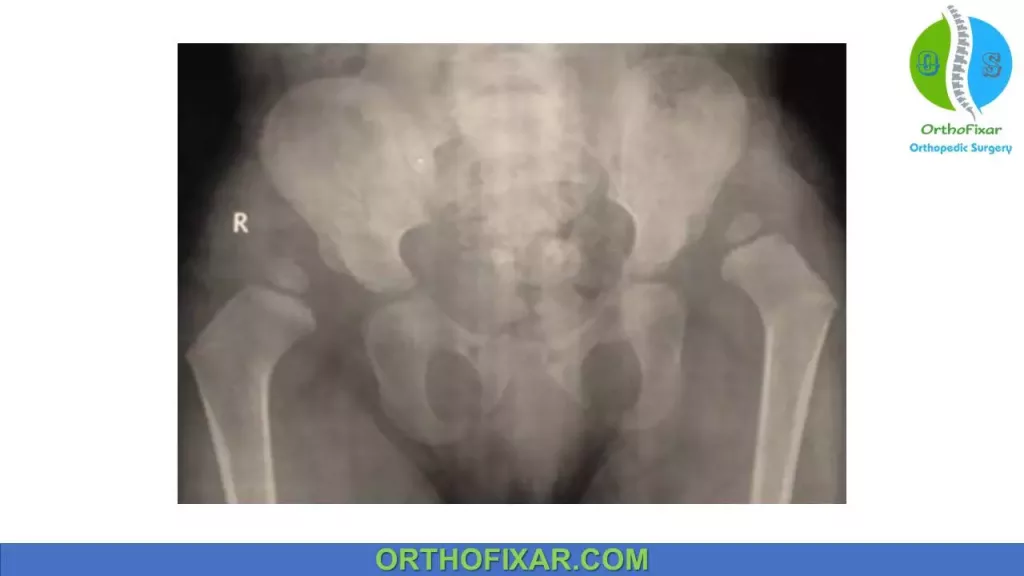
Etiology
The etiology of DDH is felt to be multifactorial, including both mechanical and physiological factors.
In utero, the hip is in a position of flexion and abduction that results in a tightened iliopsoas tendon and anterior–lateral orientation of the acetabulum.
The tight iliopsoas may push the femoral head out posteriorly with hip extension during kicking. The labrum (cartilaginous rim of the acetabulum) becomes everted and flattened.
The acetabulum and femoral head develop rapidly in the neonatal period. When the acetabulum and femoral head are in the correct position, each reinforces the development of the other by this physical contact:
- If the hip is not concentrically reduced, it will develop in a dysplastic manner.
- If the hip reduces spontaneously within a few days, hip development usually proceeds normally.
In contrast, if a subluxation or dislocation persists, the femoral head becomes flattened on the posteromedial surface, the acetabulum becomes shallow and dysplastic, and femoral anteversion gradually increases. In addition, the muscles surrounding the hip may shorten and contract.
Risk factors
Several risk factors should arouse suspicion of Developmental Dysplasia of the Hip:
- Breech positioning.
- Female sex.
- Positive family history.
- Postnatal Positioning (swaddling with the hips in extension).
- Racial Predilection (whites and Native Americans).
- Firstborn child.
- Ligamentous laxity
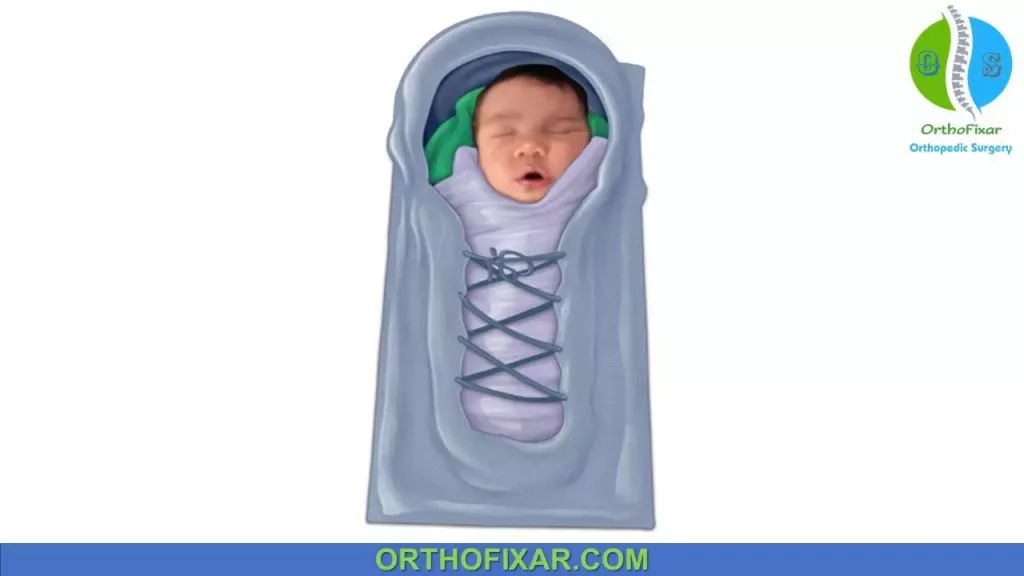
See Also: Developmental Dysplasia of the Hip Risk Factors
Associated Abnormalities
DDH is associated with multiple congenital deformities:
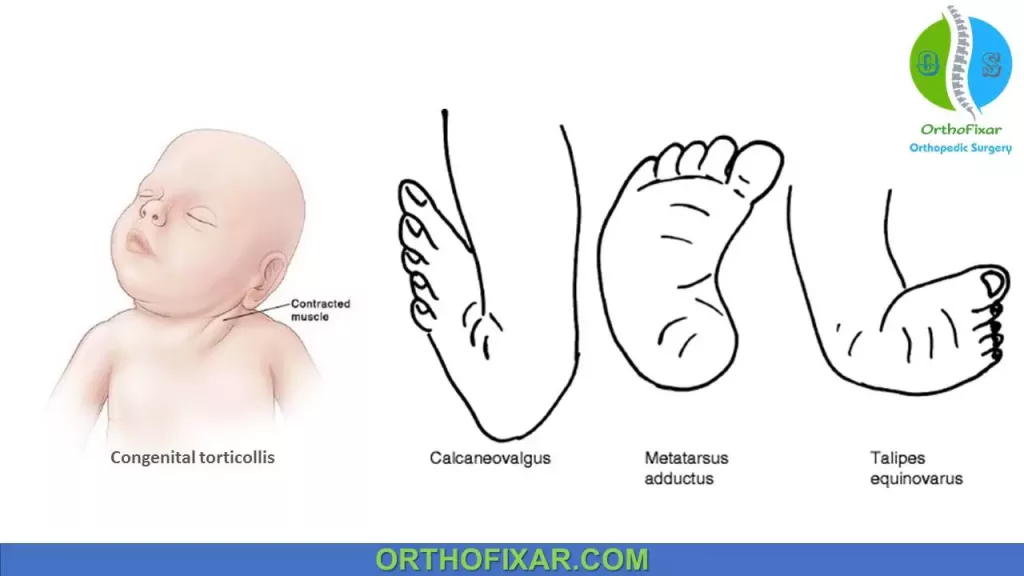
- Congenital torticollis: found in 8% , Boys more than girls.
- Metatarsus adductus.
- Talipes calcaneovalgus.
- Clubfoot deformity (Controversial): Screening hip physical examination and ultrasound evaluations for infants with clubfoot deformity is recommended.
DDH Diagnosis & Clinical Evaluation
Physical examination & diagnosis of Developmental dysplasia of the hip (DDH) varies based on the age of the child:
Newborns (<6 months old):
- The infant should be calm, relaxed, and pacified during the examination, and only one hip should be examined at a time.
- Barlow test dislocates a dislocatable hip while Ortolani test reduces a dislocated hip.
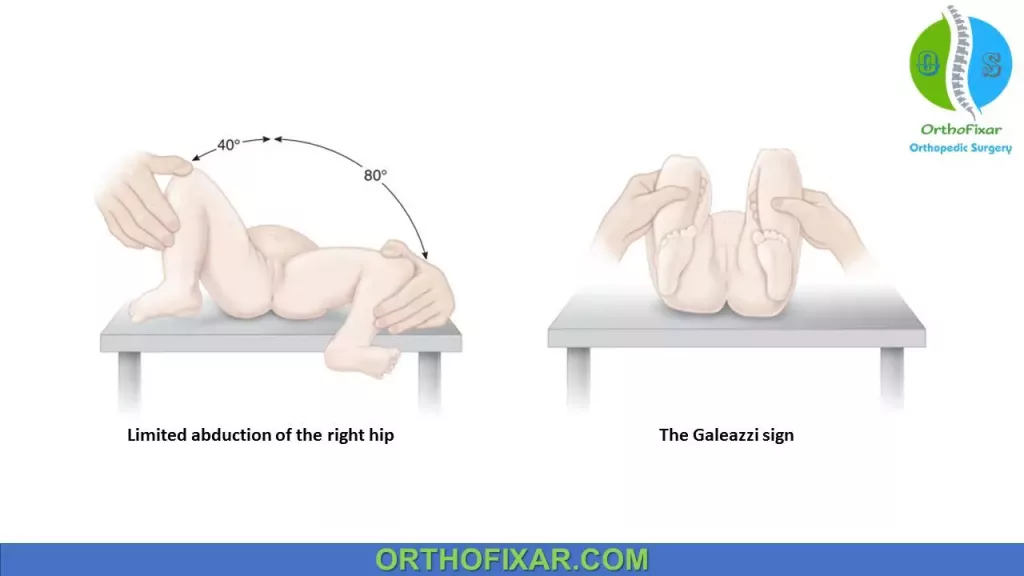
- Galeazzi sign: limb length discrepancy due to a unilateral dislocated hip with hip and knee flexed at 90 degrees.
Three phases are commonly recognized in Barlow / Ortolani test:
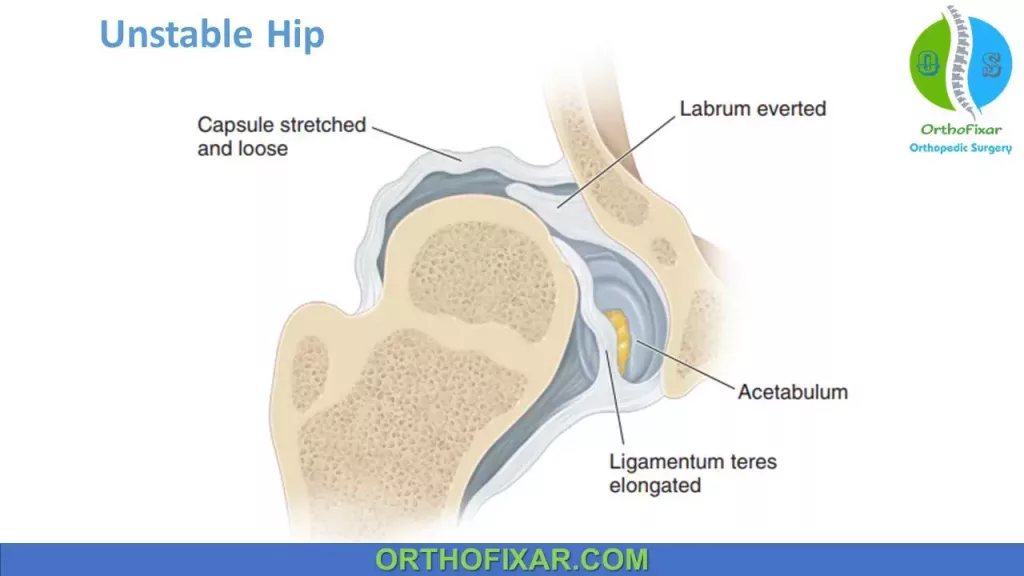
- Dislocated: Positive result of Ortolani test early, negative result of Ortolani test late, when femoral head cannot be reduced.
- Dislocatable: positive result of Barlow test.
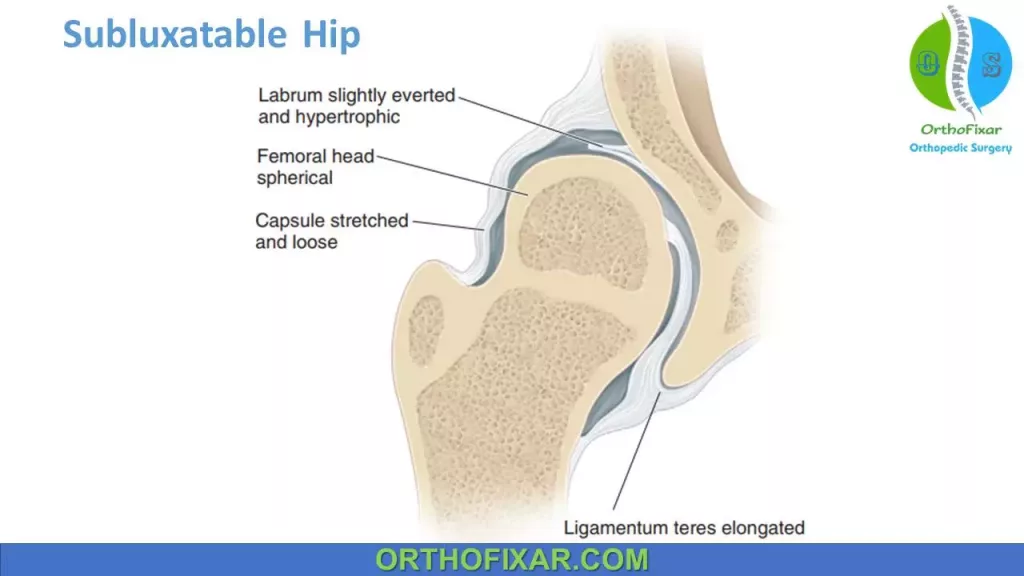
- Subluxatable: suggestive result of Barlow test.
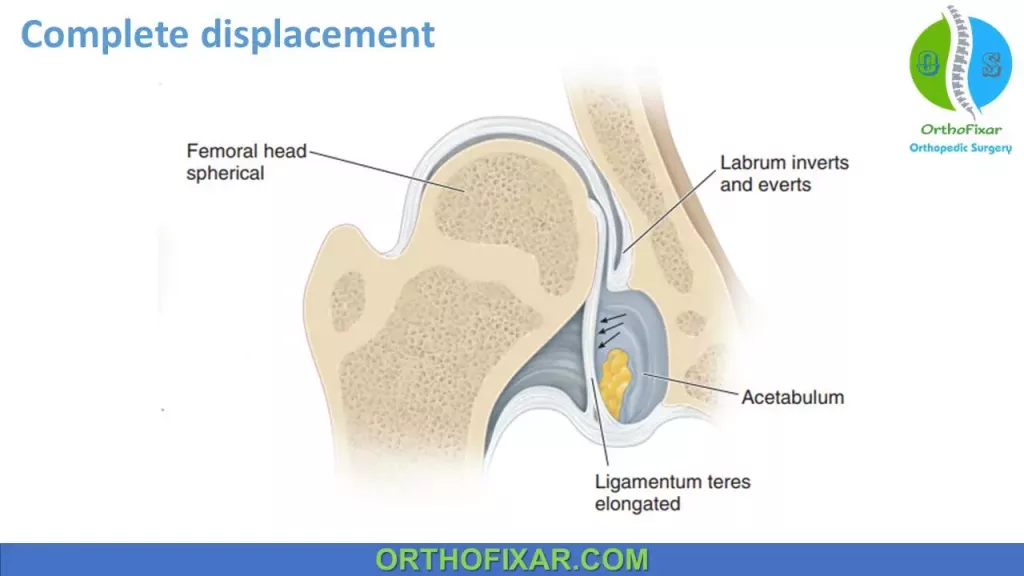
Children > 3 months:
- Limitation of hip abduction in the affected hip as the laxity resolves and stiffness becomes more clinically evident.
- Predominate of leg length discrepancy.
- Asymmetrical skin folds: This sign is not always reliable because normal children may have asymmetrical skin folds and children with dislocated hips may have symmetrical folds.
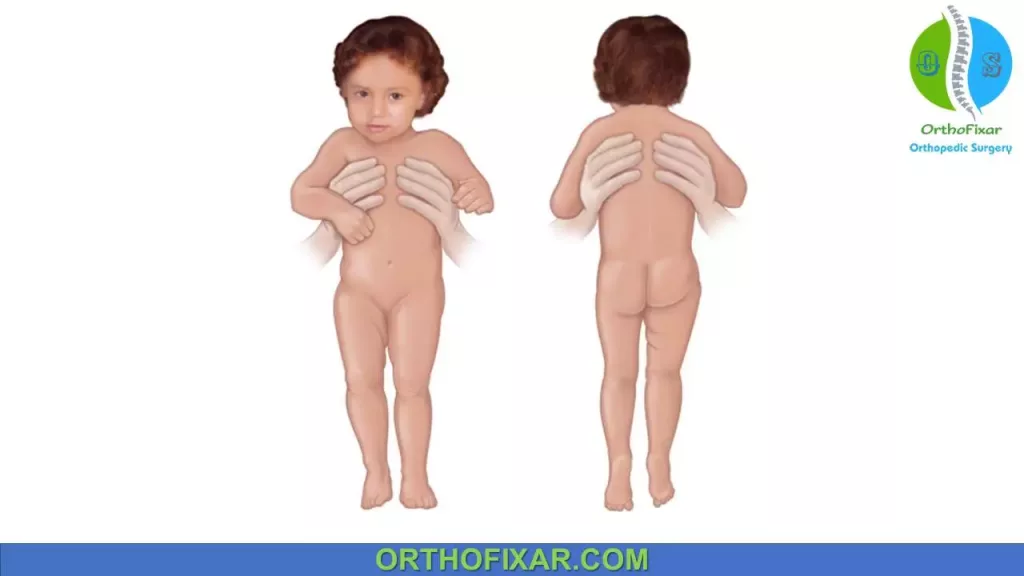
Walking child > 1 year:
- Waddling gait (bilateral dislocation).
- Trendelenburg gait (unilateral dislocation).
- Lumbar lordosis: due to hip contractures resulting from bilateral dislocations.
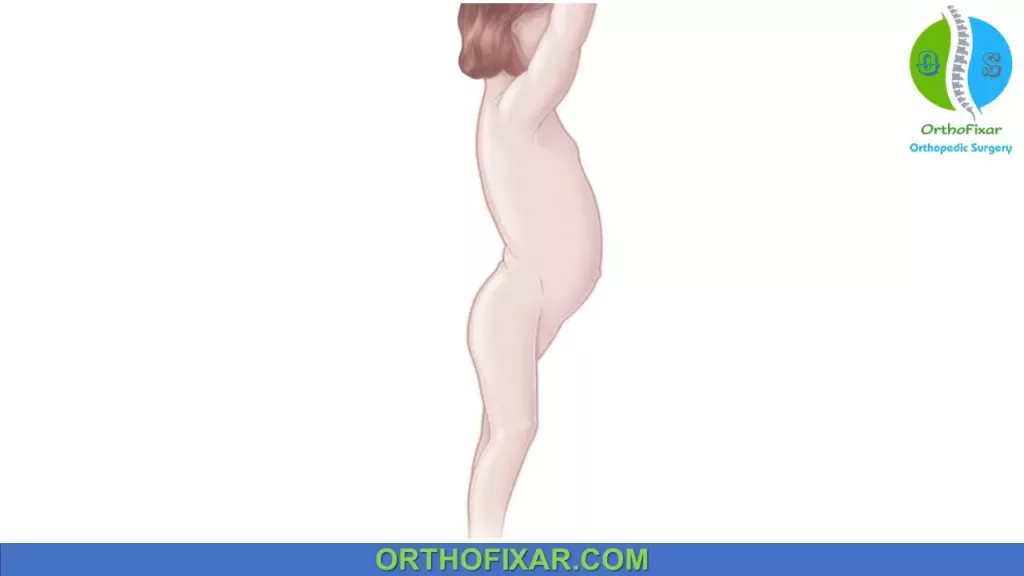
See Also: Hip joint Special Tests
Imaging Evaluation
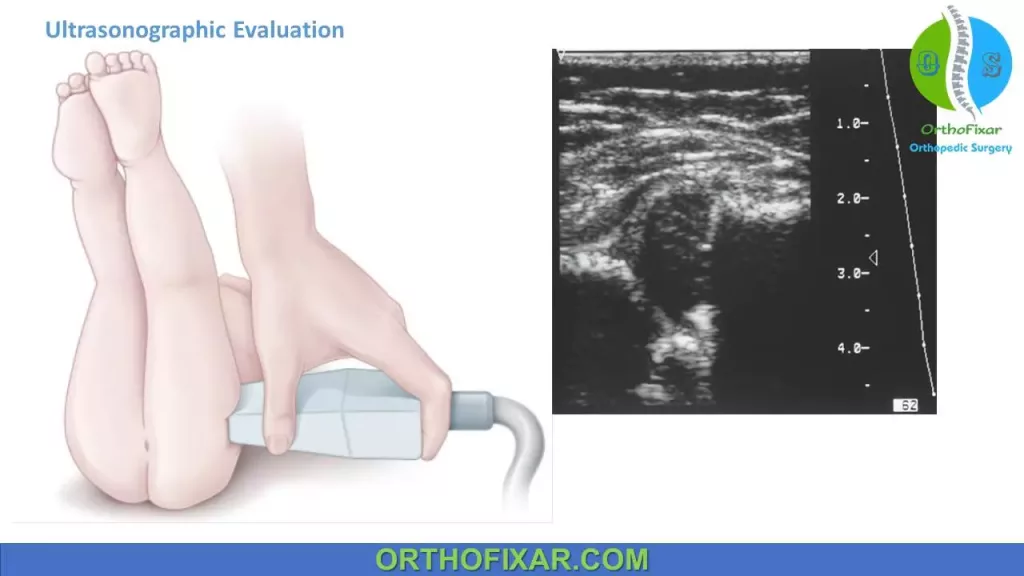
Dynamic Ultrasonography:
Dynamic ultrasonography is useful for making the diagnosis of developmental dysplasia of the hip (DDH) in young children before ossification of the femoral head (which occurs at age 4-6 months). It’s also useful for assessing reduction in a Pavlik harness and diagnosing acetabular dysplasia or capsular laxity.
Ultrasonography accuracy is dependent on examiner skill.
Ultrasound findings before 6 weeks of age can be questionable because of ligamentous laxity in the early newborn period; treatment before 6 weeks of age should be based on physical examination rather than ultrasound findings alone.
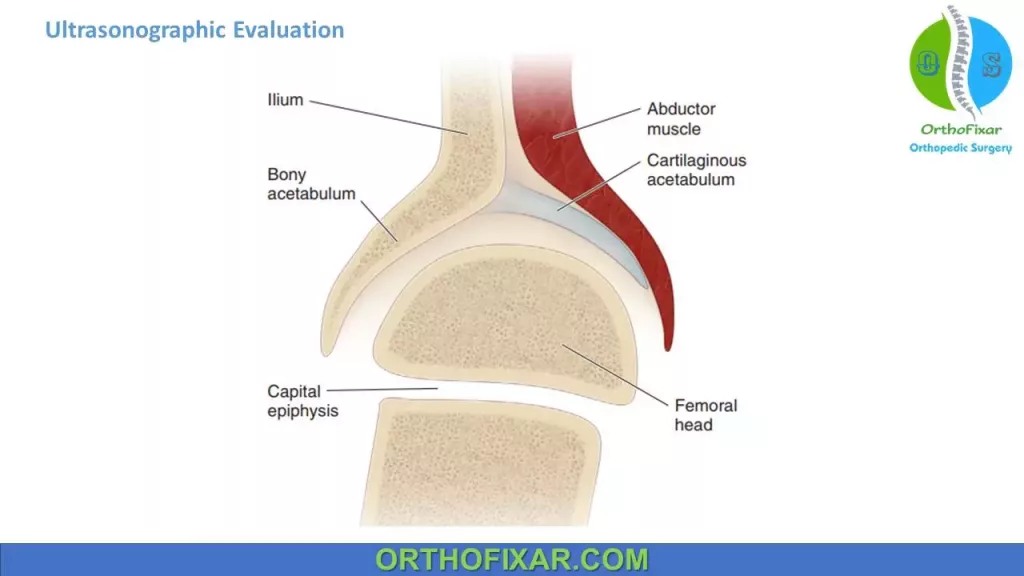
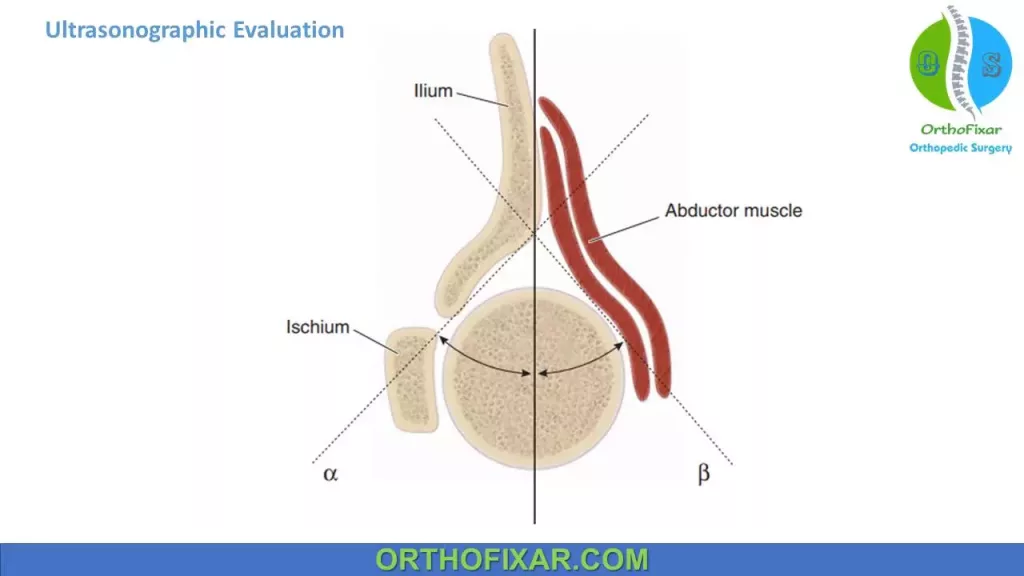
Ultrasonography Angles:
Angle α :
- It is formed by the intersection of the baseline and the acetabular roof line.
- Normal is less than 60 degrees.
Angle β:
- It is formed by the intersection of the baseline and the inclination line.
- Normal is less than 55 degrees.
Radiographic:
It’s used in older children (after age of 6 months when the femoral head begins to ossify).
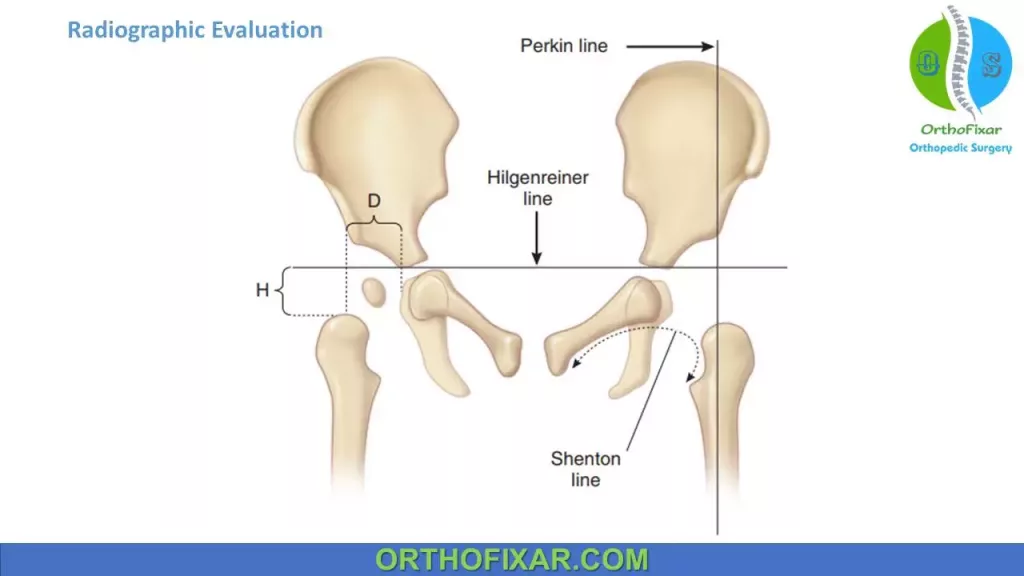
Measurements:
The most commonly used lines of reference are the:
- Vertical line of Perkins.
- Horizontal line of Hilgenreiner.
- Both used to assess the position of the femoral head.
- Shenton line is disrupted in an older child with a dislocated hip.
Normally, the femoral head lies within the inner lower quadrant of the reference lines noted by Perkins and Hilgenreiner.
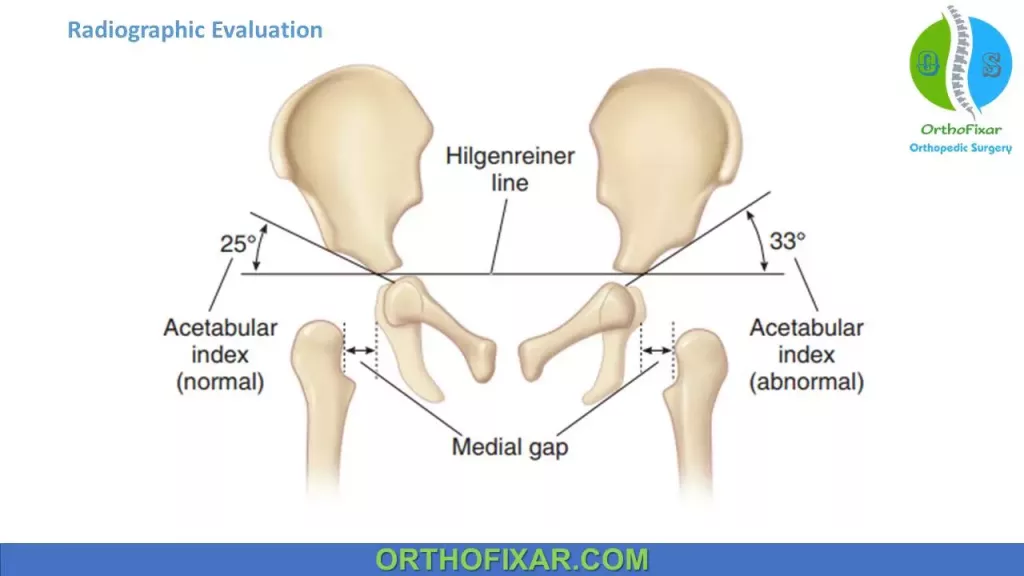
Acetabular index (AI):
Angle formed by a line drawn from point on the lateral triradiate cartilage to point on lateral margin of acetabulum and Hilgenreiners line
AI should be less than 25° in patients older than 6 months.
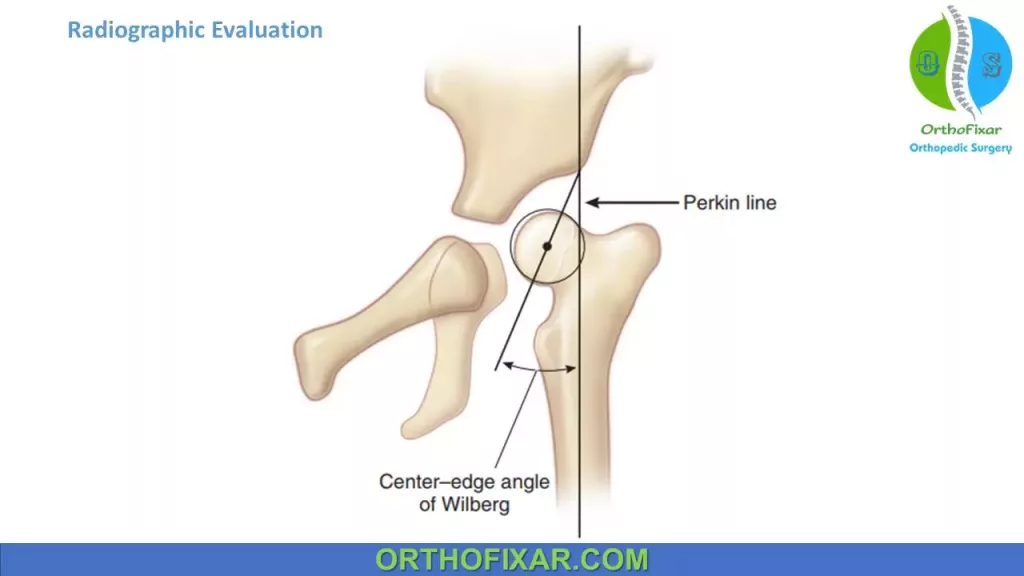
The Wilberg center–edge angle:
The Wilberg center–edge angle, which is the angle that is formed between the Perkin line and a line drawn from the lateral lip of the acetabulum through the center of the femoral head.
This angle, which is a useful measure of hip position in older children, is considered normal if it is more than 10 degrees in children between the ages of 6 and 13 years. It increases with age.
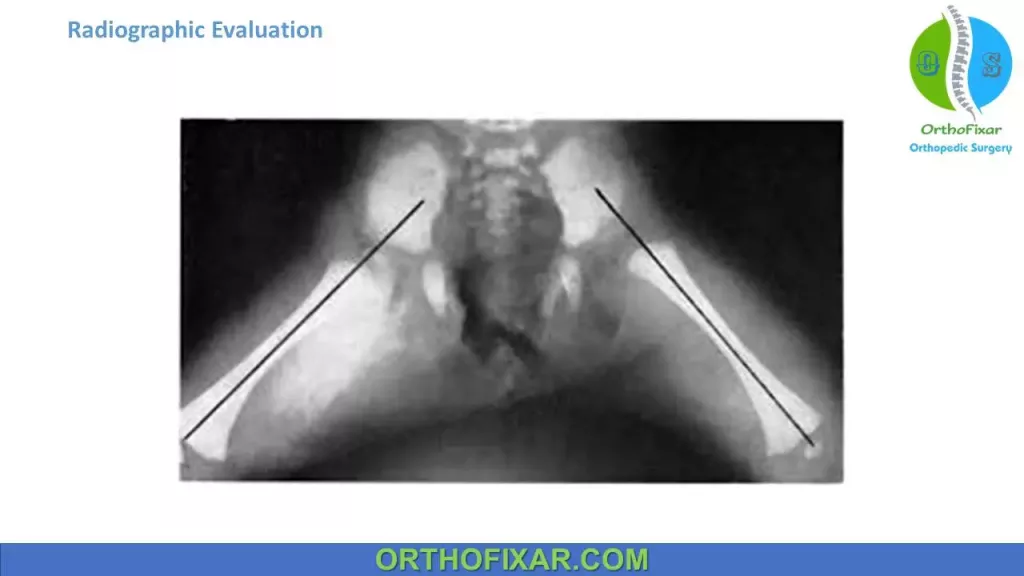
Von Rosen view:
Von Rosen view is a helpful radiographic projection, in which both hips are abducted, internally rotated, and extended.
In the normal hip, an imaginary line extended up the femoral shaft intersects the acetabulum. When the hip is dislocated, the line crosses above the acetabulum.
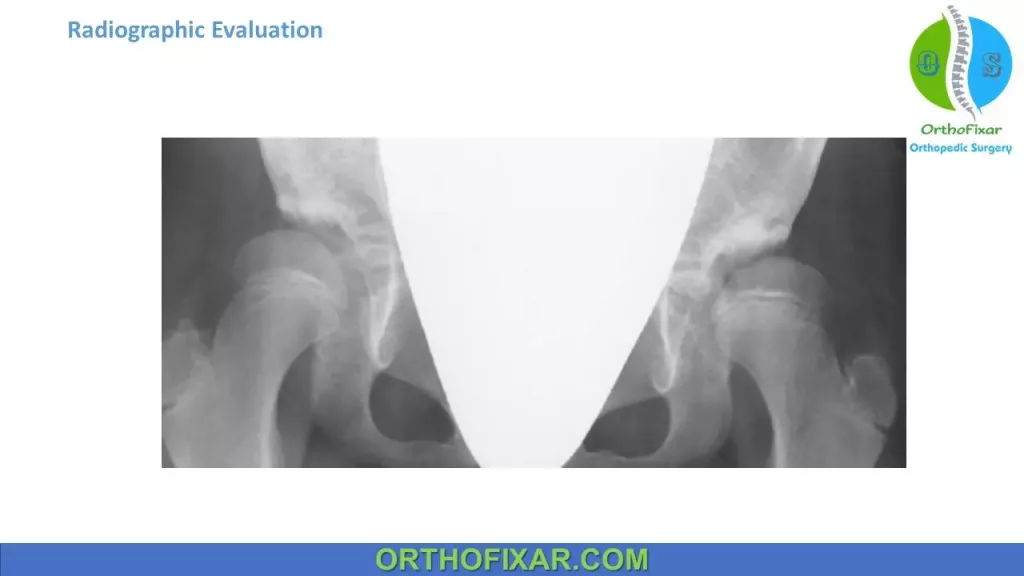
Acetabular Teardrop:
The acetabular teardrop figure, as seen on an anteroposterior (AP) radiograph of the pelvis, is formed by several lines.
It is derived from the wall of the acetabulum laterally, the wall of the lesser pelvis medially, and a curved line inferiorly, and it is formed by the acetabular notch.
The teardrop appears between 6 and 24 months of age in a normal hip and later in a dislocated hip.
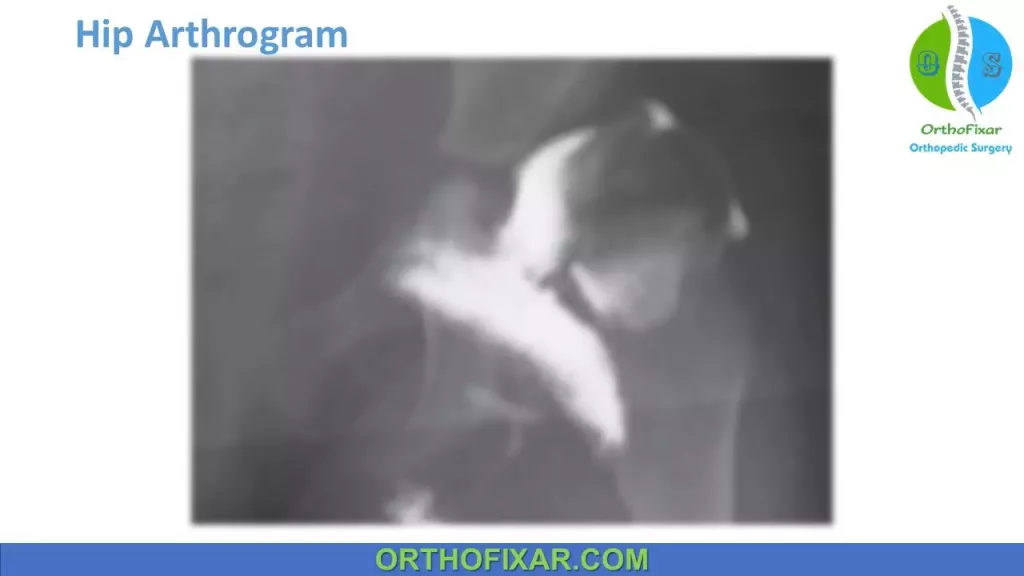
Arthrography:
Arthrography is used to help judge closed reduction and possible blocks to reduction in the treatment of Developmental Dysplasia of the Hip.
CT & MRI:
Useful after closed reduction to determine concentric reduction.
DDH Treatment
DDH Treatment is based on the child’s age:
Birth to 6 months:
Hips with normal exam but abnormal ultrasound findings Need a close follow-up, repeated ultrasound should be done at age 6 weeks, with treatment if continued signs of dysplasia.
Barlow-positive hips (reduced but dislocatable) should be watched closely. Many authors advocate treating with Pavlik while observing.
Ortolani-positive hips (dislocated but reducible): Should be treated with Pavlik harness.
Follow up check reduction after 3 weeks on ultrasonography:
- If the hip is Not reduced: consider transition to rigid abduction orthosis vs. closed reduction and spica casting.
- If the hip is reduced: continue Pavlik Harness until findings of examination and ultrasonography are normal.
Pavlik Harness:
Position of the hip is about 100 degrees of flexion and mild abduction (the human position). This position should be within the “safe zone” of Ramsey (between maximum adduction before redislocation and excessive abduction, which increases risk of avascular necrosis [AVN]). Excessive flexion may result in transient femoral nerve palsy.
Congenital hip dysplasia treatment with Pavlik harness is contraindicated in teratologic hip dislocations.
The Pavlik harness is usually worn 23 hours a day for at least 6 weeks after a reduction has been achieved and then an additional 6 to 8 weeks part time (nights and during naps).
Several series have documented the results of harness treatment. A review of a large European series of patients found that 95% of initially dysplastic hips were normal after treatment.
Risk factors for Pavlik Harness failure:
- Patient older than age 7 weeks at initiation of treatment.
- Bilateral dislocations.
- Absent Ortolani sign.
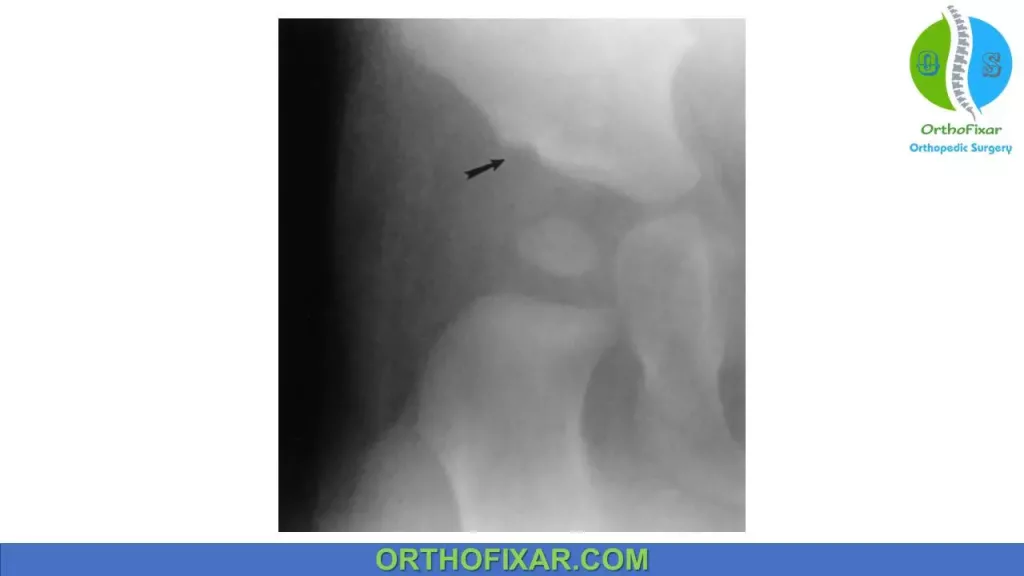
As the harness is discontinued, another AP radiograph is obtained to assess hip reduction and acetabular development. A notch above the acetabulum often appears after the hip is reduced, and this finding is usually followed by improved acetabular development. Acetabular development may be enhanced by abduction splinting, but controlled studies have not been conducted to confirm the efficacy of this common practice.

6 to 18 months:
Closed reduction and spica casting w/out Percutaneous adductor tenotomy.
Post-reduction CT or MRI scan is used to confirm concentric reduction. If closed reduction fails then open reduction is considered.
18 months to 3 years:
Developmental dysplasia of the hip surgery with open reduction and spica casting is indicated in this age group.
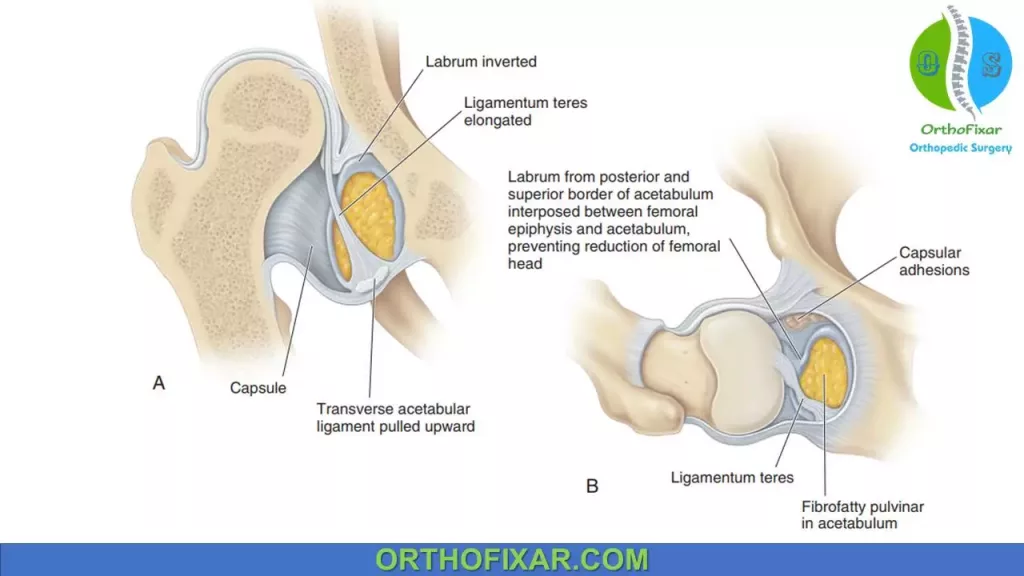
Obstacles to reduction in developmental dysplasia of the hip:
- Transverse acetabular ligament.
- Pulvinar.
- In-folded labrum.
- Inferior capsular restriction.
- Psoas tendon.
3 to 8 years:
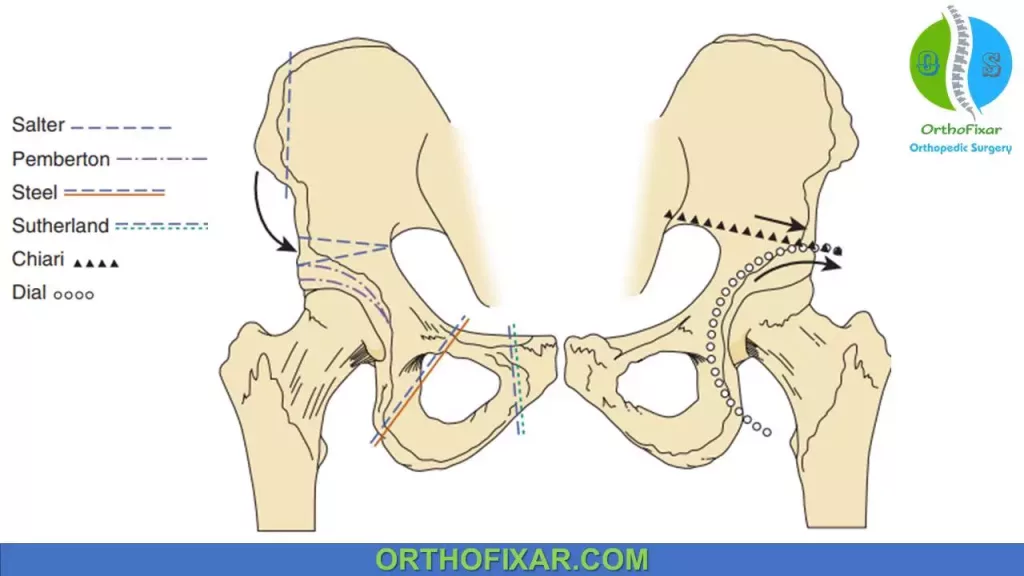
Pelvic Osteotomy: Salter, Dega, Pemberton, or Staheli procedures.
Older than 8 years:
Pelvic Osteotomy:
If the growth plate is open:
- Triple (Steele) Osteotomy.
- double pelvic (Southerland) Osteotomy.
- Staheli procedure
If the growth plate is closed:
- Ganz and Chiari procedures.
Adult Patient:
Total hip arthroplasty is indicated.
See Also: Hip Joint Osteoarthritis
Pelvic Osteotomy in treatment of developmental dysplasia of the hip:
| OSTEOTOMY | PROCEDURE | REQUIREMENT | INDICATIONS |
|---|---|---|---|
| Femoral | Intertrochanteric osteotomy (Varus derotation osteotomy) | Concentric reduction before the age of 8 years | – High neck-shaft angle – hip subluxation; – usually performed in patients with cerebral palsy |
| Salter | Open-wedge osteotomy through ileum | Concentric reduction before the age of 8 years | – Acetabular dysplasia without posterior wall loss; – redirection osteotomy |
| Pemberton | Through acetabular roof to triradiate cartilage; does not enter sciatic notch | Concentric reduction before the age of 8 years | – Acetabular dysplasia with a patulous cup; – volume-reducing osteotomy |
| Dega | Through lateral ilium above acetabulum to triradiate cartilage; incomplete cuts through innominate bone | Concentric reduction; favored in those with posterior acetabular deficiency | Acetabular dysplasia with patulous cup; – volume-reducing; – favored in neuromuscular dislocations with posterior deficiency |
| Sutherland (double) | Salter and pubic osteotomy | Concentric reduction Open triradiate cartilage | – More severe acetabular dysplasia; – redirection procedure |
| Steel (triple) | Salter and osteotomy of both rami | Concentric reduction Open triradiate cartilage | – Most severe acetabular dysplasia; – redirection procedure |
| Ganz | Periacetabular osteotomy | Surgeon’s experience Closed triradiate cartilage | Acetabular dysplasia in a skeletally mature patient |
| Chiari | Through ilium above acetabulum (makes new roof) | Non-reconstructable acetabulum | Salvage procedure for asymmetric incongruity |
| Shelf | Slotted lateral acetabular augmentation | Non-reconstructable acetabulum | Salvage procedure for asymmetric incongruity |
References
- Tachdjian Pediatric Orthopaedics 5th Edition Book.
- Millers Review of Orthopaedics, 7th Edition Book.
- Campbel’s Operative Orthopaedics 13th edition book.
- Mark Dutton, Pt . Dutton’s Orthopaedic Examination, Evaluation, And Intervention, 3rd Edition Book.
- Grill F, Bensahel H, Canadell J, Dungl P, Matasovic T, Vizkelety T. The Pavlik harness in the treatment of congenital dislocating hip: report on a multicenter study of the European Paediatric Orthopaedic Society. J Pediatr Orthop. 1988 Jan-Feb;8(1):1-8. doi: 10.1097/01241398-198801000-00001. PMID: 3335614. Pubmed
- Nandhagopal T, De Cicco FL. Developmental Dysplasia Of The Hip. 2021 Jul 18. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 33085304. Pubmed