Master Homans Sign test for DVT detection, includes step-by-step technique, accuracy and clinical interpretation. Evidence-based guide by certified physicians
Homans Sign is used to check for deep vein thrombosis (DVT) which causes calf pain. It’s sometimes called dorsiflexion sign. This sign was first described by John Homans in 1941 who was an American surgeon.
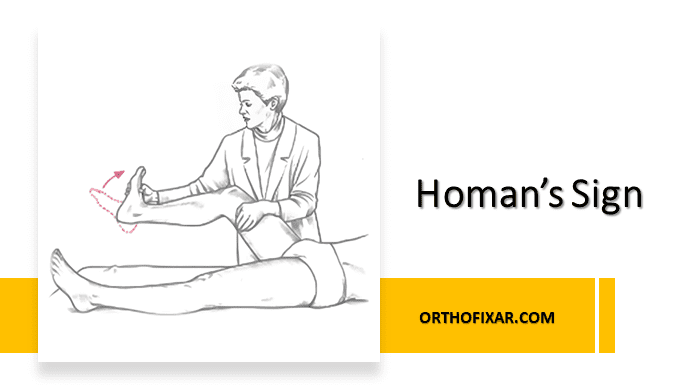
How do you Perform the Homan’s sign?
The Homans Sign test is performed with the patient in supine position. The examiner lifts the affected leg and rapidly dorsiflexes the patient’s foot with the knee extended. This maneuver is repeated with the patient’s knee flexed while the examiner simultaneously palpates the calf.
See Also: Thomas Test
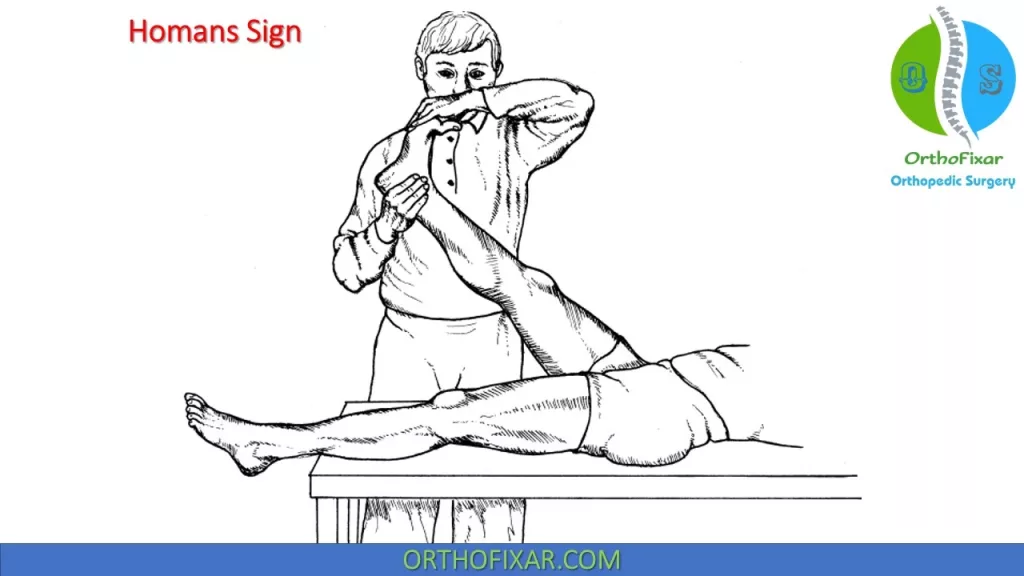
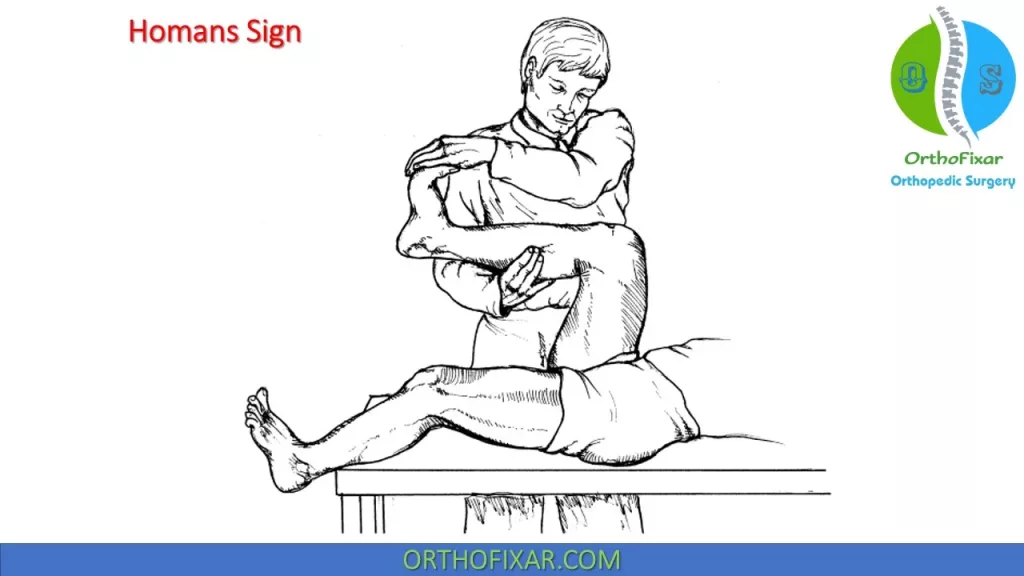
Positive Homans Sign
Homans Sign (DVT) is positive if pain is occurring upon dorsiflexion of the foot with the knee extended and flexed, this indicates deep vein thrombosis (DVT).
The explanation of the Homans sign is that the passive, abrupt and forced dorsiflexion of the ankle with knee flexion causes mechanical traction on the posterior tibial vein. This traction stimulates the pain sensitive structures in the lower limb.
See Also: Deep Venous Thrombosis (DVT)
Pain may also be elicited on palpation of the calf in conjunction with the passive stretch.
A positive finding indicates a life-threatening condition that should be addressed by appropriate medical personnel immediately
Accuracy & Releability
The sensitivity of homans sign for DVT has been questioned because deep vein thrombosis may not always produce an abnormal Homans test.
Homans sign test sensitivity and specificity is considered low as a DVT Test; but it can be of value if used in addition to more accurate diagnostic procedures like ultrasonography and venography 2.
- Sensitivity: 10-54%
- Specificity: 39-89%
In one study involving control subjects and patients with lower limb thrombosis, phlebography was used to evaluate certain clinical parameters, one of which was Homan’s sign. The results showed that all the clinical signs were inconsistent. Homans sign test was seen in only 1/3rd of patients with actual thrombosis. On the other hand, it was seen in 21% of subjects without thrombosis as well.
Homans sign though unreliable holds great historical importance. Thus it continues to be practiced in medical colleges and private physician clinics across the world because of its easy technique and simple demonstrability.
See Also: DVT Tests
Notes:
Calf pain with the knee extended can also be caused by intervertebral disk disease (radicular symptoms) or muscle contractures.
Obviously, injury to the gastrocsoleus complex may also be aggravated by Homans test.
Another case that is seen in women who after chronically wearing high heels start wearing flat shoes. In these women, sometimes due to mechanical traction in the lower limb, a positive Homans sign test can be demonstrated.
The performance of the Homans sign test may increase the risk of producing a pulmonary embolism (PE).
More accurate diagnostic DVT Tests other than Homans sign include:
- Contrast venography,
- Doppler and B-mode ultrasound,
- Venous duplex imaging,
- Impedance plethysmography,
- I-125 fibrinogen uptake.
FAQs
What is Homans Sign?
Homans Sign is a clinical test used to help detect deep vein thrombosis (DVT), a condition that causes blood clots in the deep veins of the legs. It is sometimes called the dorsiflexion sign and was first described by American surgeon John Homans in 1941.
How is the Homans Sign test performed?
The patient lies in a supine (on the back) position.
The examiner lifts the affected leg and quickly dorsiflexes the foot with the knee extended.
The maneuver is repeated with the knee flexed while simultaneously palpating the calf.
What indicates a positive Homans Sign?
A positive test occurs when the patient experiences pain during dorsiflexion of the foot, whether the knee is extended or flexed. This pain may also be felt when the examiner palpates the calf. A positive sign suggests possible DVT, which requires urgent medical attention.
How does Homans Sign cause pain?
Forced dorsiflexion of the ankle stretches the posterior tibial vein. This mechanical traction stimulates pain-sensitive structures in the lower limb, which can indicate the presence of a thrombus.
How accurate is Homans Sign for diagnosing DVT?
Homans Sign has low sensitivity and specificity:
Sensitivity: 10–54%
Specificity: 39–89%
It may appear in patients without DVT and can be absent in patients with DVT. Therefore, it is not reliable as a sole diagnostic test but can be used alongside more accurate methods such as ultrasonography or venography.
Are there any risks associated with the Homans Sign test?
Yes, performing the test may increase the risk of dislodging a clot, potentially causing a pulmonary embolism (PE).
What other conditions can cause calf pain similar to a positive Homans Sign?
Intervertebral disk disease (radicular pain)
Muscle contractures
Injury to the gastrocnemius or soleus muscles
Mechanical traction in the lower limb, sometimes seen in women who switch from high heels to flat shoes
Why is Homans Sign still practiced?
Despite its low reliability, Homans Sign remains popular in medical education and clinics due to its easy technique and demonstrability.
What are more accurate tests for DVT than Homan’s Sign?
Contrast venography
Doppler and B-mode ultrasound
Venous duplex imaging
Impedance plethysmography
I-125 fibrinogen uptake
Reference
- McGee, Steven (2012). Evidence-Based Physical Diagnosis. Philadelphia, USA: Saunders. pp. 472–473.
- Ambesh P, Obiagwu C, Shetty V. Homans sign for deep vein thrombosis: A grain of salt? Indian Heart J. 2017 May-Jun;69(3):418-419. doi: 10.1016/j.ihj.2017.01.013. Epub 2017 Jan 23. PMID: 28648447.
- Shafer N, Duboff S. Physical signs in the early diagnosis of thrombophlebitis. Angiology. 1971 Jan;22(1):18-30. doi: 10.1177/000331977102200105. PMID: 4925428.
- Mathewson M. A Homan’s sign is an effective method of diagnosing thrombophlebitis in bedridden patients. Crit Care Nurse. 1983 Jul-Aug;3(4):64-5. PMID: 6554175.
- Levi M, Hart W, Büller HR. Fysische diagnostiek–het teken van Homans [Physical examination–the significance of Homan’s sign]. Ned Tijdschr Geneeskd. 1999 Sep 11;143(37):1861-3. Dutch. PMID: 10526599.
- Pini M, Ria L, Pattacini C, Tagliaferri A, Poti R. Il segno di Homans rivisitato: è attendibile la diagnosi clinica di trombosi venosa profonda? [Homan’s sign revisited: is the clinical diagnosis of deep venous thrombosis reliable?]. Recenti Prog Med. 1984 Jul-Aug;75(7-8):650-7. Italian. PMID: 6505364.
- Urbano, FL: Homans’ sign in the diagnosis of deep vein thrombosis. Hosp Physician, March:22, 2001.
- Homans J. Thrombophlebitis in the legs. New Engl J Med. 1938;218:594–599.
- Homans J. Diseases of the veins. New Engl J Med. 1944;231:51–60.
- McGee, Steven (2012). Evidence-Based Physical Diagnosis. Philadelphia, USA: Saunders. pp. 472–473.
- Clinical Tests for the Musculoskeletal System 3rd Edition.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Sarvdeep S. Dhatt, Sharad Prabhakar – Handbook of Clinical Examination in Orthopedics.