Distal Radius Fractures is the most common fracture encountered by orthopedic trauma surgeons accounting for 17.5% of all adult fractures, with around 120,000 fractures per year in the United Kingdom and 607,000 annually in the United States.
Distal Radius Anatomy
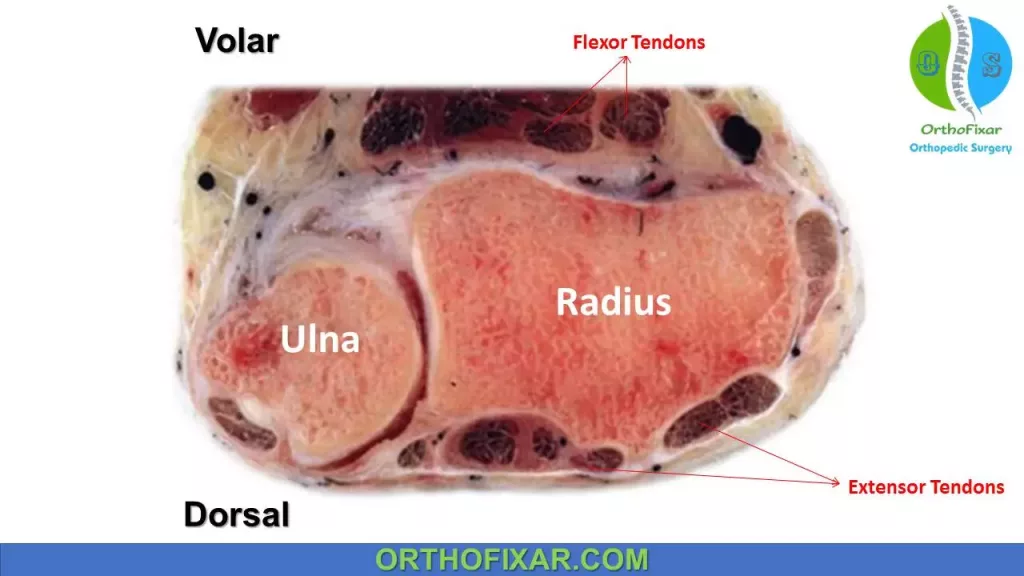
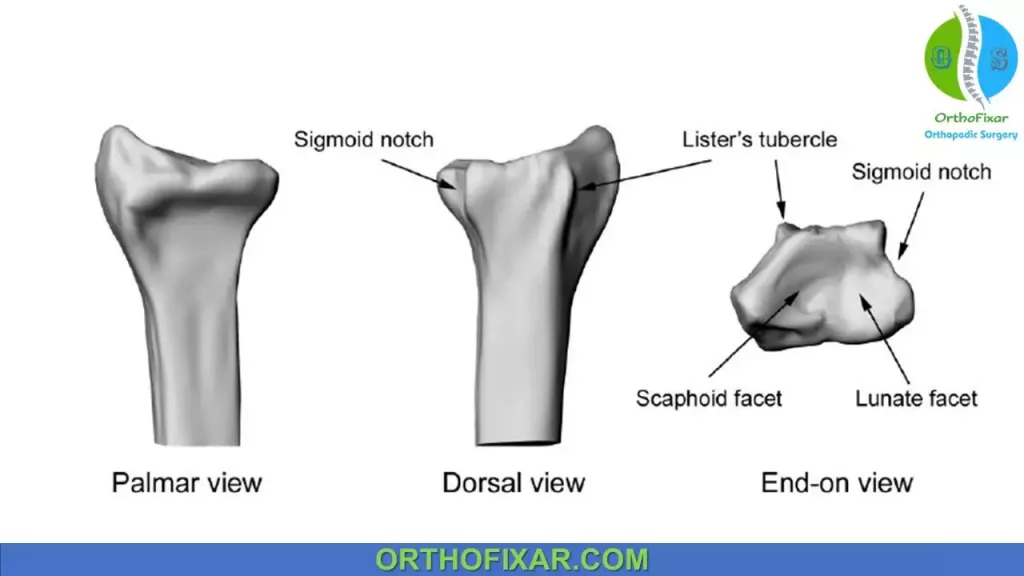
The distal radius articular surface is biconcave, which contains the scaphoid, and lunate facets. The radius articulates with ulna at sigmoid notch forming the Distal radioulnar joint (DRUJ). Normally the distal radius bears 80% of axial load in the normal wrist.
Reversal of the normal palmar tilt results in load transfer onto the ulna and TFCC; the remaining load is then borne eccentrically by the distal radius and is concentrated on the dorsal aspect of the scaphoid fossa.
Lister tubercle is a small dorsal prominence (a landmark for dorsal approach to wrist).
Metaphysis is a thin cortex, vulnerable to bending forces.
Brachioradialis muscle insertion on the styloid process acts as a major deforming force in distal radius fractures.
Numerous ligamentous attachments exist to the distal radius; these often remain intact during distal radius fracture, facilitating reduction through “ligamentotaxis.” The volar ligaments are stronger and confer more stability to the radiocarpal articulation than the dorsal ligaments.
Epidemiology
High-energy injury occurs in young patients, and accounts for around 10% of all wrist fractures, while low-energy injury occurs in old patients, it is the cause of the majority of distal radius fractures with 66% to 77% of fractures being related to a fall from standing height.
The majority (57% to 66%) of fractures are extra-articular, between 9% and 16% are reported as partial articular and 25% to 35% as complete articular fractures.
Men who sustain distal radius fractures are significantly younger than women. The average age of all distal radius fractures in adults has been reported to be between 57 and 66 years with females being on average in their 60s and men in their 40s.
Risk Factors for Distal Radius Fractures
- Decreased bone mineral density,
- Female sex,
- White race,
- Family history,
- Early menopause.
Mechanism of Injury
Common mechanisms of injury in younger individuals include:
- Falls from a height,
- Motor vehicle accident,
- Injuries sustained during athletic participation.
In elderly individuals, distal radial fractures may arise from low-energy mechanisms, such as a simple fall from a standing height and as such are considered fragility fractures.
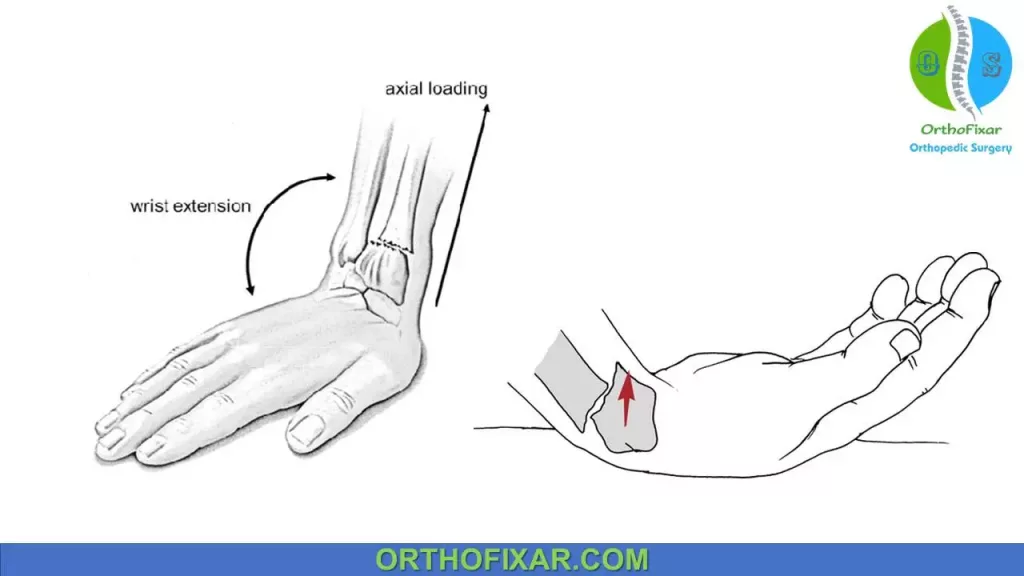
The most common mechanism of injury of distal radius fractures is a fall onto an outstretched hand with the wrist in dorsiflexion.
Fractures of the distal radius are produced when the dorsiflexion of the wrist varies between 40 and 90 degrees. The radius initially fails in tension on the volar aspect, with the fracture propagating dorsally, whereas bending moment forces induce compression stresses resulting in dorsal comminution. Cancellous impaction of the metaphysis further compromises dorsal stability.
Additionally, shearing forces influence the injury pattern, often resulting in articular surface involvement.
High-energy injuries (e.g., vehicular trauma) may result in significantly displaced or highly comminuted unstable fractures to the distal radius.
The different characteristics of fractures of the distal radius are generally agreed to be influenced by:
- Position of the hand at the time of impact,
- The type of surface with which it makes contact,
- The velocity of the force.
- The quality and strength of the bone of the distal radius will influence the severity of the fracture.
Associated injuries
The main injuries associated with distal radius fractures are those to the interosseous ligaments of the carpus and to the triangular fibrocartilage complex (TFCC).
1. Interosseous Ligament Injury:
Interosseous ligament injury associated with fractures of the distal radius is predominantly scapholunate and lunatotriquetral injury.
Scapholunate injury has been reported to occur in between 4.7% and 46% of distal radius fractures, while Lunatotriquetral injury is less common with prevalences between 12% and 34%.
The severity of these injuries has been graded arthroscopically by Geissler from grade 1 to grade 4:
- Grade 1 injuries are the least severe with attenuation or hemorrhage,
- grades 2 and 3 are increasing incongruity of the ligament,
- grade 4 is gross instability with sufficient disruption to allow passage of an arthroscope from radiocarpal to midcarpal joints.
The diagnosis of ligament injury can be made from static radiographs of the distal radius in the more severe cases. The diagnosis can be difficult when associated with a distal radius fracture. Arthroscopy is probably the best method but is expensive and may subject the patient to an unnecessary procedure.
An increased risk of interosseous ligament injury has been demonstrated where there is more than 2 mm of positive ulnar variance and in intra-articular fractures.
The significance of interosseous ligament tears to the outcome of distal radius fractures is unclear. It has been suggested that undetected lesions are a cause of ongoing pain.
2. Triangular Fibrocartilage Complex (TFCC) Injury:
TFCC injury is commoner than interosseous ligament injury being reported in 39% to 82% of cases. The majority are peripheral avulsions and may be associated with ulnar styloid fractures, the presence of which increases the risk of a TFCC tear.
Surgery to repair TFCC tears has good reported results, although the indications for surgical treatment of these injuries have not yet been clearly defined.
Clinical Evaluation
Pain and swelling around the wrist are invariable features.
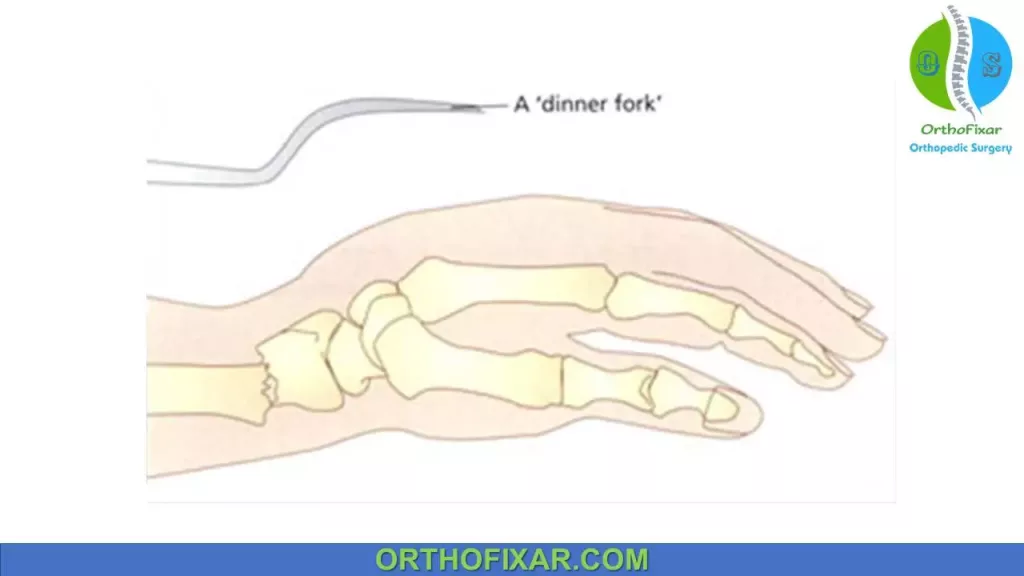
Visible deformity if there is displacement, the classical dinner fork or silver fork deformity is caused by dorsal displacement of the carpus secondary to dorsal angulation of the distal radius. The reverse deformity is seen in volar displaced fractures. The hand may be radially deviated and if there is shortening of the radius the ulna will be prominent.
Look for paresthesia or numbness in the fingers to exclude any median or ulnar nerve injury. The distal radius fractures may be complicated by acute compartment syndrome and the symptoms and signs of this condition should also be sought.
The skin should be inspected to rule out any open wounds, which most commonly occur on the ulnar side.
Evidence of pain elsewhere in the limb should be sought to diagnose an ipsilateral injury
Radiographic Evaluation
Recommended views in radiographic evaluation of distal radius fractures include:
- posteroanterior (PA),
- lateral,
- oblique x-ray views.
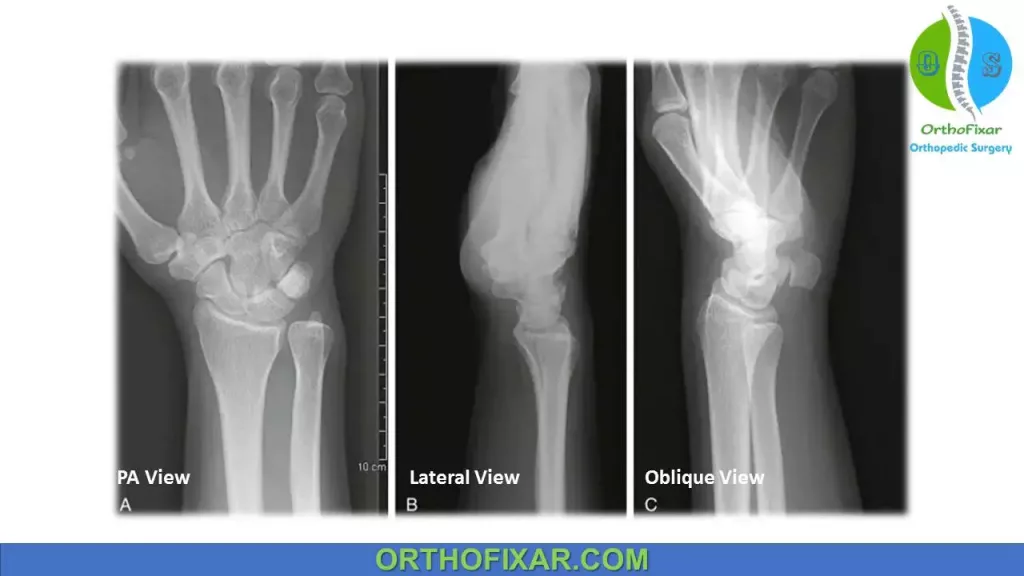
A number of radiologic measurements quantifying the orientation of the distal radius are used:
| Measurement | Description | Normal Value | Acceptable criteria |
|---|---|---|---|
| Dorsal/palmar tilt | On a true lateral view, a line is drawn connecting the most distal points of the volar and dorsal lips of the radius. The dorsal or palmar tilt is the angle created with a line drawn along the longitudinal axis of the radius. | 11 degrees | dorsal angulation <5° or within 20° of contralateral distal radius |
| Radial length | On the PA radiograph. It is the distance in millimeters between a line drawn perpendicular to the long axis of the radius and tangential to the most distal point of the ulnar head and a line drawn perpendicular to the long axis of the radius and at the level of the tip of the radial styloid | 13 mm | <5 mm shortening |
| Radial inclination | On the PA view the radius inclines toward the ulna. This is measured by the angle between a line drawn from the tip of the radial styloid to the medial corner of the articular surface of the radius and a line drawn perpendicular to the long axis of the radius. | 23 degrees | change <5° |
| Articular stepoff | Seen on PA view. | congruous | <2 mm stepoff |
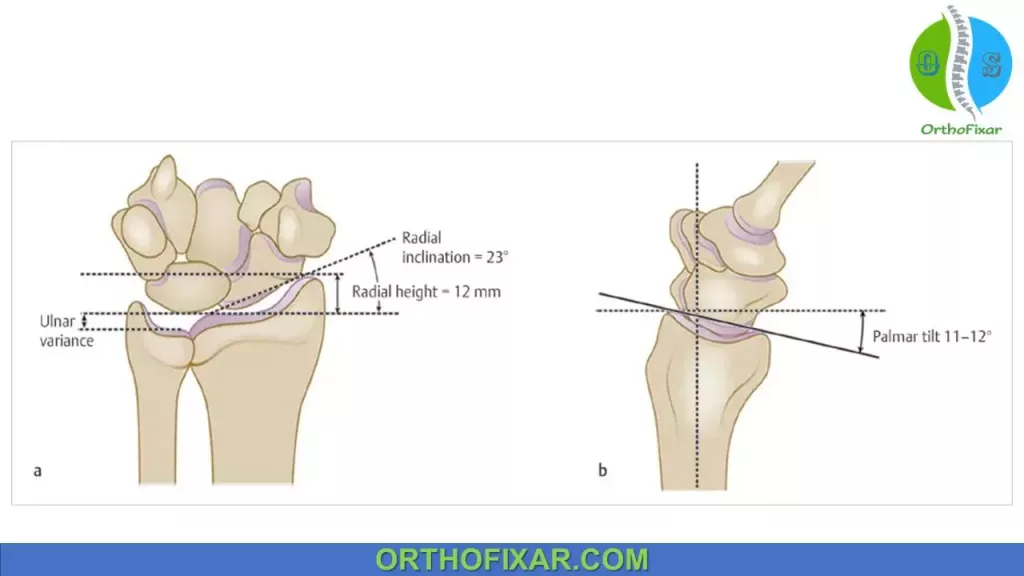
Ulnar variance:
This is a measure of radial shortening and should not be confused with the measurement of radial length.
Ulnar variance is the vertical distance between a line parallel to the medial corner of the articular surface of the radius and a line parallel to the most distal point of the articular surface of the ulnar head, both of which are perpendicular to the long axis of the radius.
Carpal malalignment:
There are two types of carpal malalignment associated with fracture of the distal radius. The commonest is malalignment which compensates for the tilt of the distal radius and is extrinsic to the carpus.
On a lateral view one line is drawn along the long axis of the capitate and one down the long axis of the radius. If the carpus is aligned the lines will intersect within the carpus. If not, they will intersect outwith the carpus. Carpal malalignment can also be caused by associated carpal ligament disruption.
Teardrop angle and anteroposterior (AP) distance:
The teardrop of the distal radius articular surface refers to the U-shaped outline of the volar rim of the lunate facet. It refers to the angle between the central axis of the teardrop and the central axis of the radial shaft.
Depression of the teardrop angle to less than 45 degrees indicates displacement of the lunate facet. A depressed teardrop angle may be the only evidence that reduction is incomplete and articular incongruity remains.
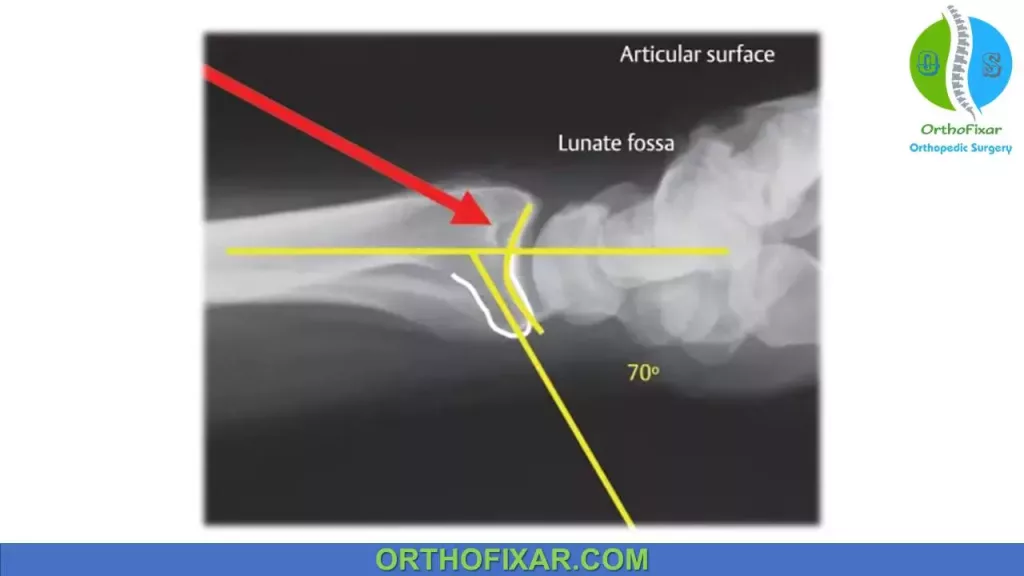
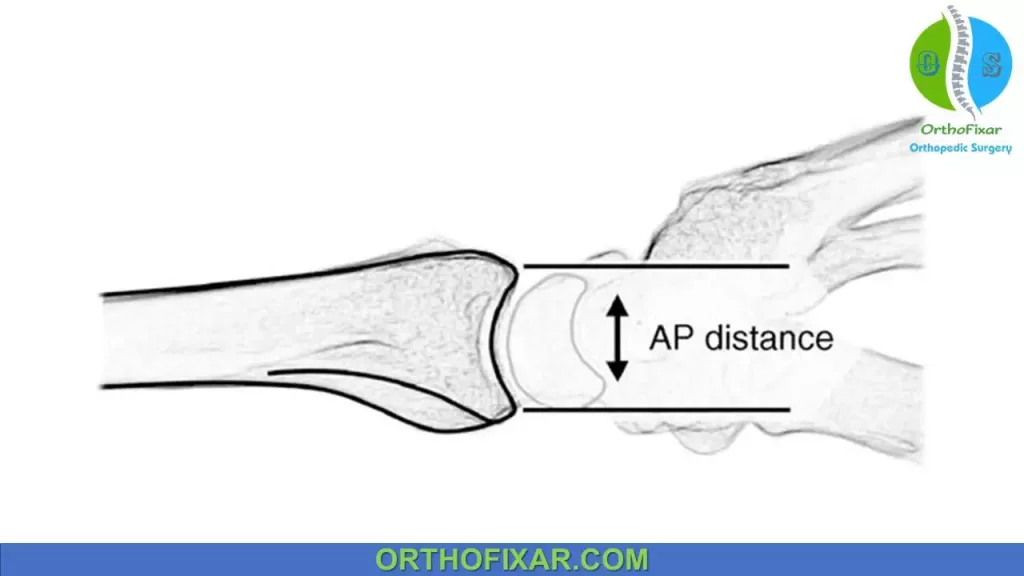
The AP distance is also a measure of articular incongruity and is defined by the distance between the apices of the dorsal and volar rims of the lunate facet.
The normal AP distance averages 19 mm on a true lateral view, but is probably best assessed by comparison with the contralateral normal wrist
Specific features should be assessed on each view of the distal radius as follows:
| Extra-articular fractures | Intra-articular fractures | |
|---|---|---|
| PA View | Radial length/ulnar variance. Extent of metaphyseal comminution. Ulnar styloid fracture location (tip/waist/base) . | Presence and orientation of articular fractures. Depression of the lunate facet. Gap between scaphoid and lunate facet. Central impaction fragments. Carpal bone assessment: Gilula’s carpal arc 1 or evidence of a scaphoid fracture. |
| Lateral View | Dorsal/palmar tilt. Extent of metaphyseal comminution. Carpal alignment. Displacement of the volar cortex. Position of the DRUJ. | Depression of the palmar lunate facet. Depression of the central fragment. Gap between palmar and dorsal fragments. Scapholunate angle for possible associated carpal injury. Teardrop angle. AP distance. |
Oblique Views:
The pronated oblique view demonstrates the radial side of the distal radius and is particularly useful for assessing radial comminution, a split or depression of the radial styloid, and for confirming the position of screws on the radial
side of the distal radius.
The supinated oblique view demonstrates the ulnar side of the distal radius and is useful for assessing depression of the dorsal lunate facet and the position of ulnar-sided screws.
Tilted Lateral View:
This is a lateral view taken with a pad under the hand to incline the radius 22 degrees toward the beam.
It provides a tangential view of the lunate facet and allows more accurate measurement of lunate facet depression and possible screw penetration into the radiocarpal joint.
Traction Views (AP and Lateral):
These views are taken with manual traction or finger traps applied after reduction and under anesthetic. They are most useful in articular fractures and allow the surgeon to plan whether closed techniques will be sufficient for treatment or whether open reduction will be necessary.
A traction view also helps to identify fracture fragments that may be obscured by the displacement of the fracture and emphasizes any disruption of Gilula’s arc in the proximal carpal row in associated interosseous ligament injury.
Contralateral Wrist (AP and Lateral):
These x-rays may be indicated prior to surgery to assess the patient’s normal ulnar variance, scapholunate angle, and AP distance, all of which vary between patients.
Computerized Tomography CT:
CT scanning is used to improve the visualization and accuracy of measurement of articular fractures in the distal radius.
Distal Radius Fracture Types
Types of distal radius fractures:
| Fractures Type | Description |
|---|---|
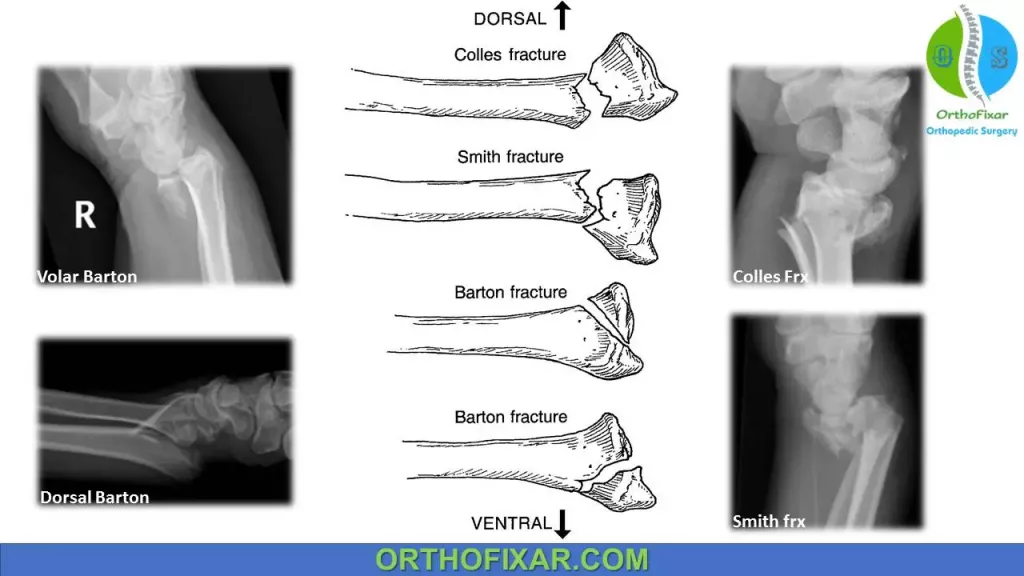
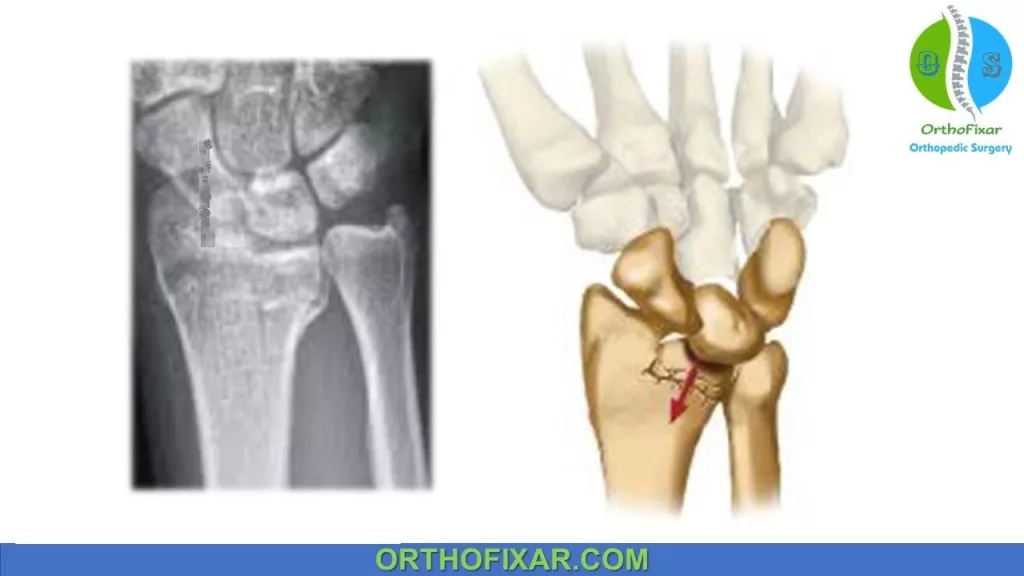
| Die-punch fracture | A depressed fracture of the lunate fossa of the articular surface of the distal radius |
| Barton fracture | Fracture dislocation of radiocarpal joint with intra-articular fracture involving the volar or dorsal lip (volar Barton or dorsal Barton fracture) |
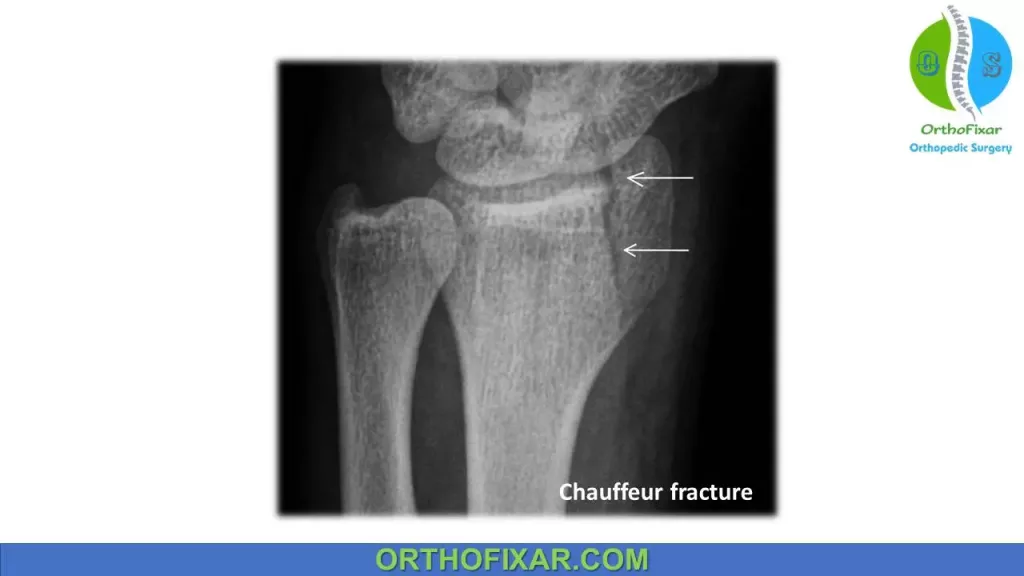
| Chauffer fracture | Radial styloid fracture |
| Colles fracture | Low energy, dorsally displaced, extra-articular fracture |
| Smith fracture | Low energy, volar displaced, extra-articular fracture |
Frykman Classification:
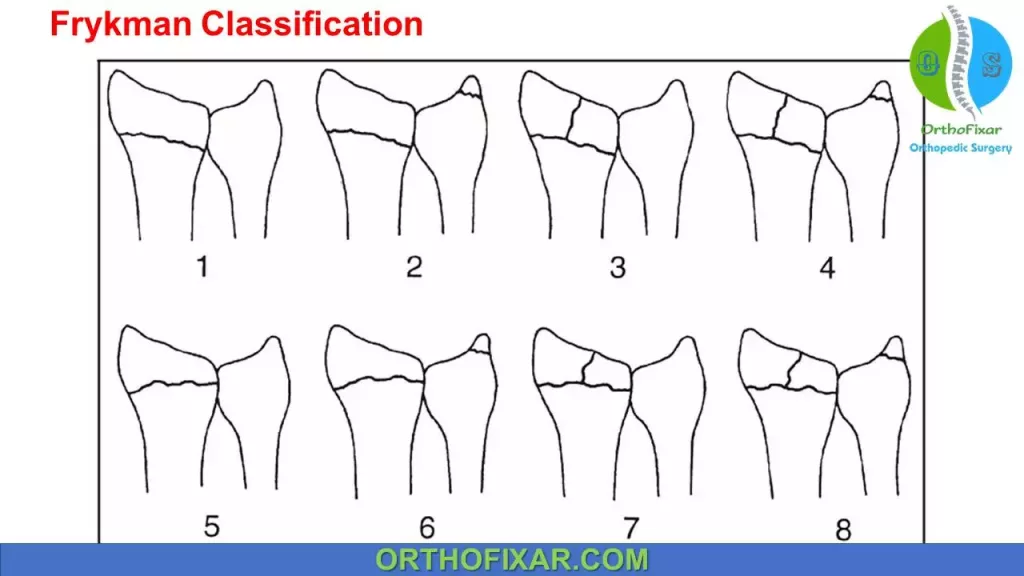
Frykman classified fractures of the distal radius concentrating on articular and ulnar (styloid or shaft) involvement. He specifically differentiated between radiocarpal and distal radioulnar joint involvement, as he believed that intra-articular involvement and ulnar involvement were the most prognostic factors:
| Type | Description |
|---|---|
| Type I | Extra-articular, no ulnar fracture |
| Type II | Extra-articular, ulnar fracture |
| Type III | Radiocarpal articular, no ulnar fracture |
| Type IV | Radiocarpal articular, ulnar fracture |
| Type V | DRUJ articular, no ulnar fracture |
| Type VI | DRUJ articular, ulnar fracture |
| Type VII | Radiocarpal and DRUJ, no ulnar fracture |
| Type VIII | Radiocarpal and DRUJ, ulnar fracture |
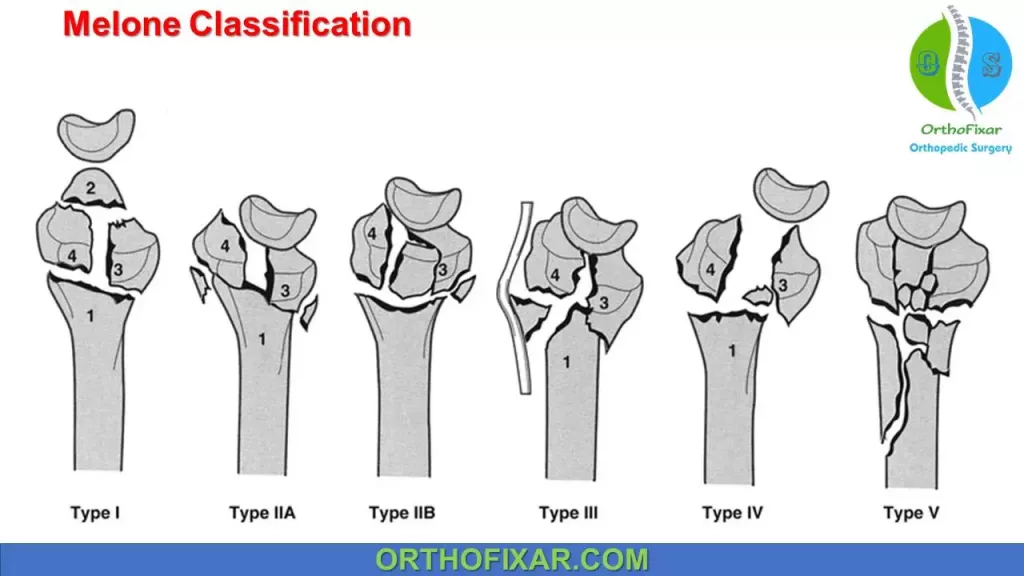
Melone Classification:
Melone classified intra-articular fractures of the distal radius by considering that each fracture consisted of four parts:
- Radial styloid,
- Dorsal medial fragment,
- Volar medial fragment,
- The radial shaft.
He termed the two medial fragments, which make up the lunate fossa the medial complex and based his classification on the position of the medial complex.
| Type | Description |
|---|---|
| Type I | Undisplaced or variable displacement of the medial complex as a unit. No comminution. Stable after closed reduction. |
| Type II | Unstable, die punch. Moderate or severe displacement of the medial complex as a unit with comminution of dorsal and volar cortices. A: Irreducible, closed. B: Irreducible, closed because of impaction. |
| Type III | As type 2 but with a spike of the radius on the volar side, which may compromise the median nerve. |
| Type IV | Split fracture, unstable. The medial complex fragments are severely comminuted with rotation of the fragments |
| Type V | Explosion injury. Severe displacement and comminution often with diaphyseal comminution |
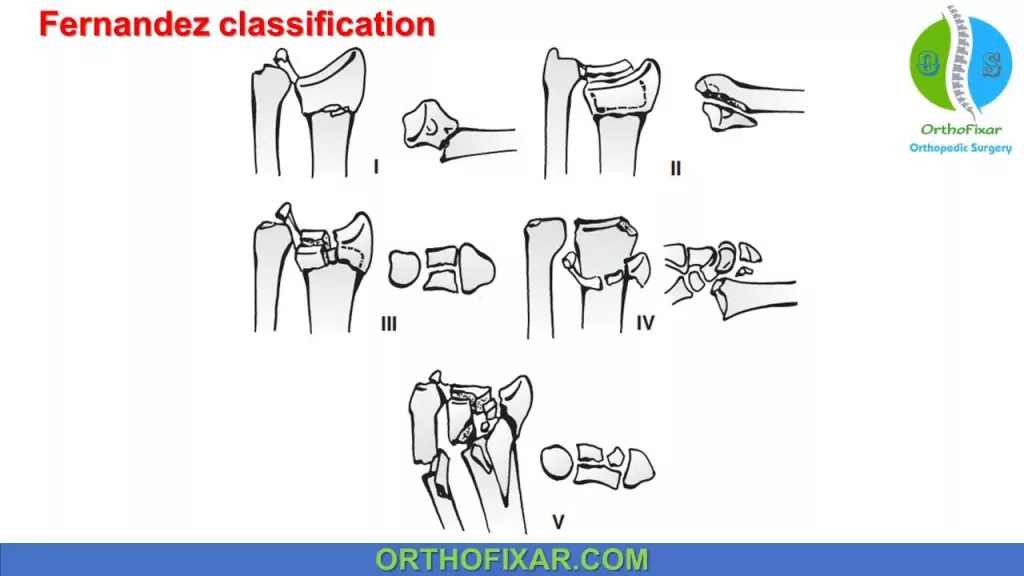
Fernandez classification:
Fernandez classification is a mechanism-based classification system:
| Type I | Metaphyseal bending fracture with the inherent problems of loss of palmar tilt and radial shortening relative to the ulna (DRUJ injury) |
| Type II | Shearing fracture requiring reduction and often buttressing of the articular segment |
| Type III | Compression of the articular surface without the characteristic fragmentation; also the potential for significant interosseous ligament injury |
| Type III | Avulsion fracture or radiocarpal fracture dislocation |
| Type IV | Combined injury with significant soft tissue involvement owing to high-energy injury |
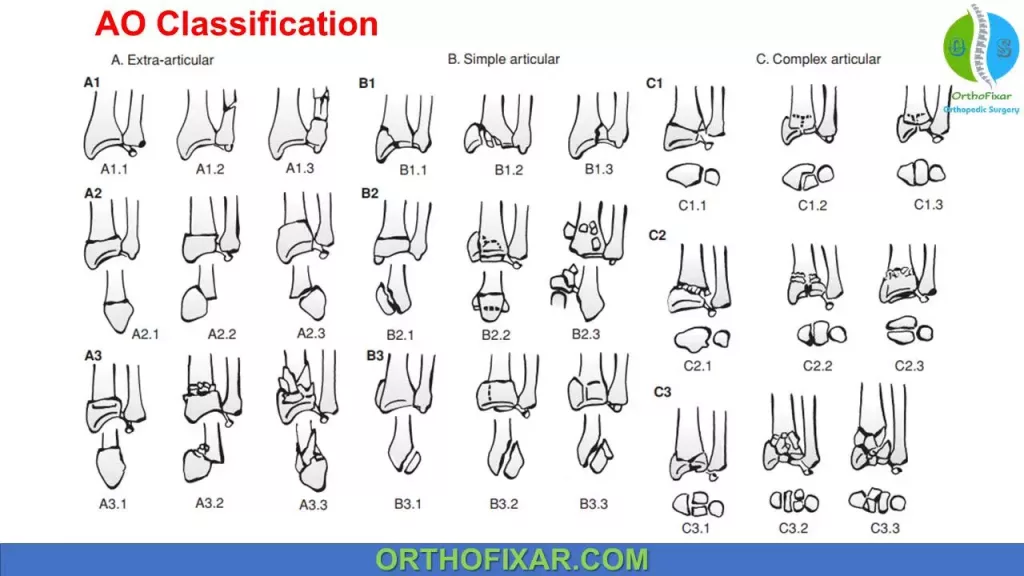
AO Classification:
This is an inclusive, alphanumeric classification and has 27 different subgroups.
Three different types are divided into 9 main groups:
- A: extra-articular,
- B: partial articular,
- C: complete articular)
27 different subtypes depending on comminution and direction of displacement.
Distal Radius Fractures Treatment
There are numerous treatment options for the management of distal radius fractures including nonoperative, external fixation, and internal fixation.
The main goals of Distal Radius Fractures treatment is:
- Restore the function of the hand and wrist.
- Maintain reduction until union.
- Prevent symptomatic posttraumatic radiocarpal osteoarthrosis.
Factors to consider before treatment include:
- age,
- medical condition,
- activity demands,
- bone quality,
- fracture stability,
- associated injuries.
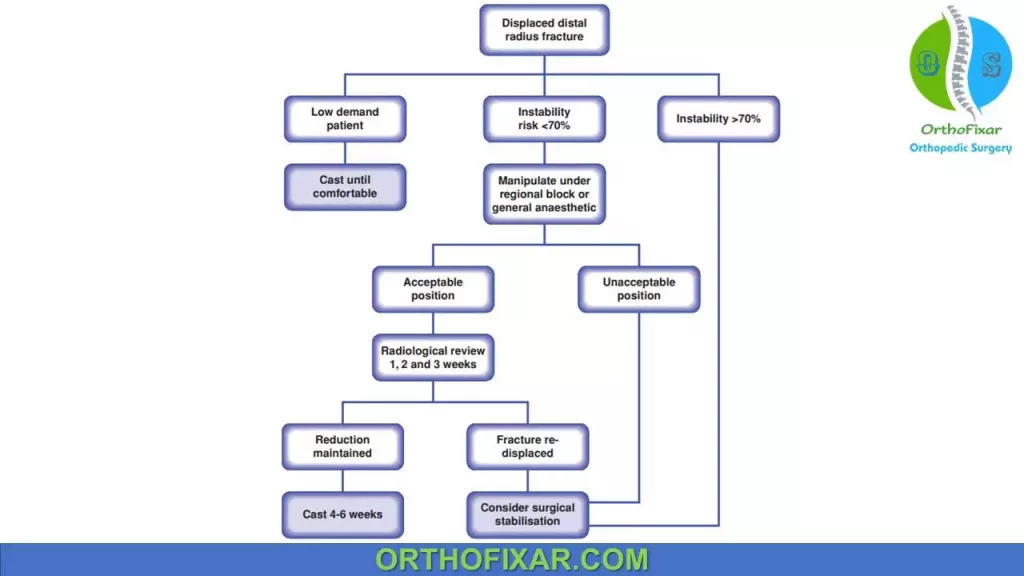
Several factors have been associated with re-displacement following closed manipulation of a distal radius fracture:
- Age: Patients over 80 years of age with a displaced fracture of the distal radius are three times more likely to have instability than those under 30 years of age.
- Initial Fracture Displacement: The greater the degree of initial displacement (particularly radial shortening), the more energy is imparted to the fracture resulting in a higher likelihood that closed treatment will be unsuccessful.
- Metaphyseal Comminution: The presence of a metaphyseal defect as evidenced by either plain radiographs or computerized tomography increases the chance of instability.
- Displacement Following Closed Treatment: This is a predictor of instability as repeat manipulation is unlikely to result in a successful radiographic outcome.
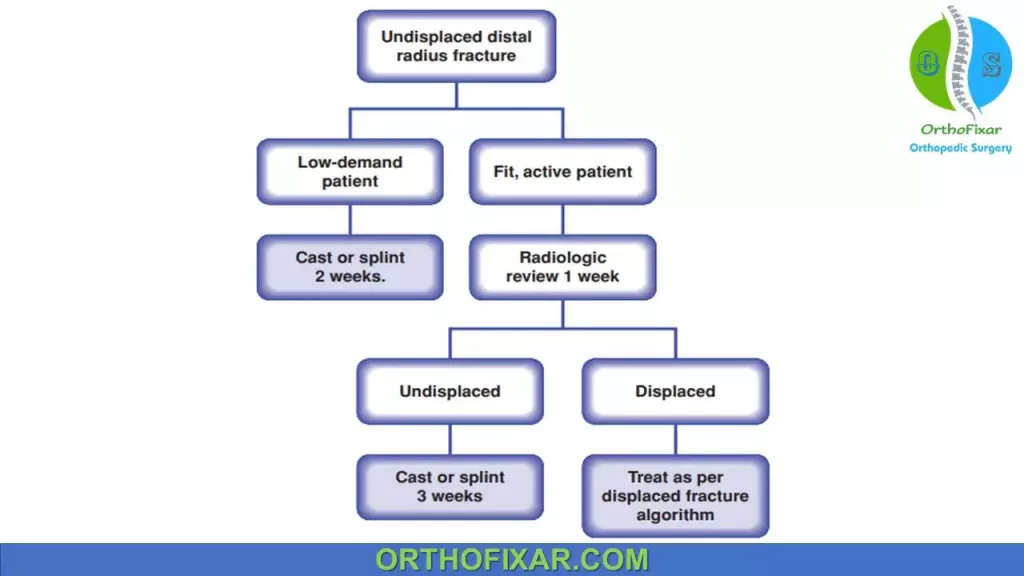
Nonoperative Treatment:
Nonoperative distal radius fracture treatment is indicated for undisplaced stable fractures or displaced fractures which are stable after reduction.
Manipulative reduction is indicated where the radiologic position falls outwith acceptable limits and nonoperative treatment is predicted to be successful, that is, if the fracture is likely to be stable.
Radiographs obtained weekly for first 3 weeks.
Postreduction benchmarks:
- Radial shortening less than 3 mm.
- Dorsal articular tilt less than 10 degrees.
- Intraarticular step-off less than 2 mm.
Immobilization for 6 to 8 weeks.
Both forearm and above-elbow casts have been used for distal radius fractures. Above-elbow casts were used because it was believed that holding the forearm in supination prevented redisplacement from the deforming force of brachioradialis. However, randomized studies have shown no benefit of above-elbow immobilization compared to forearm casts in maintaining the fracture reduction.
Operative Treatment:
There are a number of methods of operative treatment available for distal radius fractures including:
1. Closed reduction and percutaneous pinning (CRPP)
2. External fixation:
- Bridging and nonbridging techniques described
- Role in fractures with open contaminated wounds
- Difficult to restore articular alignment and volar tilt
- Overdistraction may lead to increased risk of complex regional pain syndrome (CRPS).
3. Distraction plating:
- Also termed bridge plating or “internal ex fix”
- Secured second or third metacarpal and radial shaft
- Alternative to external fixation in highly comminutedfractures or in elderly patients with severe osteoporosis.
- Disadvantage is second surgery to remove plate at 8 to 12 weeks.
4. Open reduction with internal fixation (ORIF):
- Dorsal plating: Best for dorsally displaced fractures with dorsal bony defects, disadvantage includes extensor tendon irritation or rupture from prominent hardware.
- Volar plating: Best for Smith and Barton fracture patterns but often method of choice for dorsally displaced injuries as well
Concurrent treatment of ulnar styloid fracture is not routinely necessary. No difference in multiple outcome measures when comparing patients undergoing ORIF of distal radius with and without ulnar styloid fixation Painful nonunion/DRUJ instability in small number of cases after radial fracture reduction (<10%).

Complications
- Median nerve neuropathy (CTS)
- Ulnar nerve neuropathy
- EPL rupture
- Radiocarpal arthrosis
- Malunion and Nonunion
- ECU or EDM entrapment
- Compartment syndrome
- RSD/CRPS
Vitamin C in doses of at least 500 mg/day for 50 days may decrease the incidence of CRPS in women older than age 50 treated for a distal radius fractures.
Questions by Patients:
How long does it take a distal radius fracture to heal?
Distal radius fracture usually takes a period of 4-6 weeks to heal.
Do you need physical therapy after broken wrist?
Yes for sure, after your doctor remove the splint, you will need to have a course of physical therapy by a specialist to re-gain your joint movement and muscle strength.
Why is distal radius fracture common?
Distal radius fracture is a common fracture seen in ER especially in older patients because of osteoporosis they have which makes the bones very fragile and more likely to break.
Does a distal radius fracture require surgery?
This depends on the displacement and severity of the distal radius fractures. Displaced fractures can be treated by closed reduction w/o pinning or by open reduction with plate fixation. While non-displaced fractures is treated by casting for 4-6 weeks.
References
- Geissler WB, Freeland AE, Savoie FH, McIntyre LW, Whipple TL. Intracarpal soft-tissue lesions associated with an intra-articular fracture of the distal end of the radius. J Bone Joint Surg Am. 1996 Mar;78(3):357-65. doi: 10.2106/00004623-199603000-00006. PMID: 8613442.
- Lindau T, Arner M, Hagberg L. Intraarticular lesions in distal fractures of the radius in young adults. A descriptive arthroscopic study in 50 patients. J Hand Surg Br. 1997 Oct;22(5):638-43. doi: 10.1016/s0266-7681(97)80364-6. PMID: 9752922.
- Richards RS, Bennett JD, Roth JH, Milne K Jr. Arthroscopic diagnosis of intra-articular soft tissue injuries associated with distal radial fractures. J Hand Surg Am. 1997 Sep;22(5):772-6. doi: 10.1016/S0363-5023(97)80068-8. PMID: 9330132.
- Shih JT, Lee HM, Hou YT, Tan CM. Arthroscopically-assisted reduction of intra-articular fractures and soft tissue management of distal radius. Hand Surg. 2001 Dec;6(2):127-35. doi: 10.1142/s021881040100059x. PMID: 11901458.